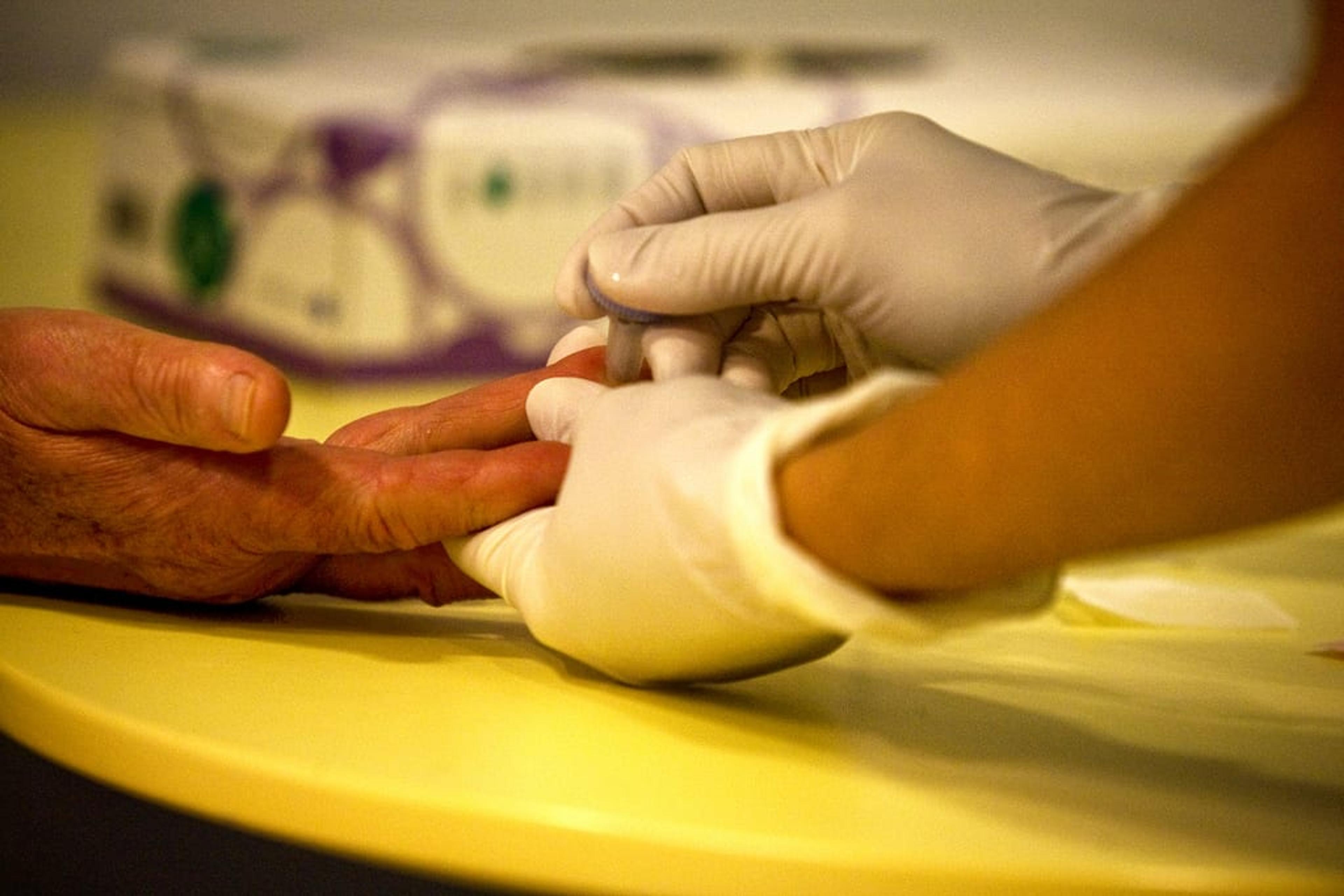
As a Henry Ford Health System nurse case manager for diabetes patients, I select the patients I see. This means stepping in to assist diabetes patients who may be in the worst phases of their disease, giving me an eye-opening look into the chronic condition that affects 29.1 million Americans. Flipping through my appointment book a few years ago, a patient immediately caught my eye both because of her young age and an out of control blood sugar level – a 43 year-old diabetic who had not been to the doctor in two years, with an A1C reading of 13.5. For those not familiar with blood sugar readings, an A1C test determines the average level of blood sugar over a three-month span – a healthy reading for a diabetic patient being anywhere under eight. After reviewing her chart I knew I had to meet Sarah. I look back on this day as one of the most memorable in my career, because although Sarah’s health journey was long, I believe I made a difference in both the quality of her health and her life entirely. When Sarah and I first met she wasn’t aware of the effects of high blood sugar on her health, so much so that wasn’t checking her levels at all. She wasn’t taking insulin, which is vital to a diabetic’s health and wasn’t taking her prescribed oral medication correctly. Her health was on a major decline and could’ve evolved into being life-threatening without immediate intervention. After our introductions and developing a rapport with Sarah, I got down to the bottom of her unwillingness to battle her condition – as a teenager, she had been diagnosed with Hodgkin’s lymphoma. In remission from this illness, she was afraid of getting news like that again. I could tell it was that experience that kept her from wanting to actively treat her diabetes. Her experience also helped to guide my relationship with her, taking everything one step at a time. The foundation of Blue Cross Blue Shield of Michigan’s Patient-Centered Medical Home program relies on collaborative care between physicians, case managers and specialists to best manage the health of a patient. This collaboration requires a sense of trust between medical professionals and patients and helps create activated patients, where individuals are active players in their health care, a part of their own team. My time with Sarah would not have been possible without this kind of integrated care supported by Blue Cross’ program. Sarah was a prime example of the importance and value of individual care management through a Patient-Centered Medical Home. Through the Patient-Centered Medical Home program, care providers can recognize when a patient isn’t following recommended health interventions and will seek to understand why as quickly as possible to get the patient back on track. A lot of the time you need to make people sit down and talk to them about their barriers to care – what’s stopping them from taking care of themselves? Most of the time, patients don’t have all the medical information and when you’re able to provide a personal experience and explain conditions in a way they understand with the help of additional medical resources and professionals, the process doesn’t seem so scary. From there, checking in with Sarah to schedule her appointments with specialists became my focus. I’d call about her follow-ups with gynecologists, endocrinologists and gastrologists. As a school teacher, her busy schedule seemed like a barrier in the beginning, but through collaborative efforts, we developed an appointment schedule revolving around her lunch hour. We would talk about her health and how to stay on track. The ultimate goal for me was to help Sarah get healthy and stay that way. Sarah’s renewed effort in her own health proved to be life-changing beyond improving her handle on diabetes. An appointment we scheduled with a gastrologist identified two polyps which were safely removed. These life-saving surgeries would never have occurred if Sarah had continued to ignore her disease. As a result of our work together, Sarah returned to her physician with an A1C reading of 7.5, administering her insulin correctly, hemoglobin returning to a normal level and a refreshed perspective on living a healthy life. Through recommended changes in her diet and exercise, I wanted her to experience what it feels like to live with diabetes in a happy, healthy state. Though Sarah and I are no longer in contact following her remission, I believe our time together was imperative to her overall wellbeing. Receiving customized care and physician collaboration through Patient-Centered Medical Homes supported by Blue Cross helped her avoid serious life-threatening illnesses. These types of trusting partnerships between medical professionals and patients are the cornerstone of medical care and of the utmost importance in the world of Michigan medicine. This post is part of a storytelling series we call, “Beyond the Card.” These stories will feature Blue Cross Blue Shield of Michigan members, employees, and communities who are making meaningful differences throughout our state. We invite you to follow Beyond the Card stories here at MIBluesPerspectives.com and through the hashtag, #BeyondtheCard on our social channels. If you have a story you would like to share, please feel free to contact us at stories@bcbsm.com. Photo credit: Oskar Annermarken





