Connecting the Dots: A Full Health Approach to Integrated Care

Dr. Amy McKenzie
| 3 min read
Dr. Amy McKenzie, MD, is vice president of clinical partnerships and associate chief medical officer at Blue Cross Blue Shield of Michigan. She is a board-certified family medicine physician. She serves on the State of Michigan Certificate of Need Commission. She graduated from Northeast Ohio Medical University and completed her residency at St. John Providence Health System in Southfield, Michigan. In 2017, she completed her MBA with a focus in medical management at the University of Massachusetts Amherst.

A behavioral health crisis has been building for years. In any given year, one in five adults will experience a diagnosable mental health condition, and more than half will go untreated. The reality is those diagnosed with a chronic condition are twice as likely to have a behavioral health condition, and vice versa. And, the health care costs for treating individuals with behavioral and chronic medical conditions are two to three times higher than for those without behavioral health conditions. Addressing the challenge takes a more comprehensive, more integrated approach — one aimed at valuing and treating behavioral and physical health together and seamlessly carving in pharmacy benefits while connecting primary and behavioral care providers; one built around a network of coordinated, multidisciplinary care models; one that favors innovative partnerships and virtual care platforms; and one that supports the full continuum of conditions, from the most severe to everyday stressors. All of these integrations are paramount to the member’s experience and overall care management.
CONFRONTING COMORBIDITY FULL ON
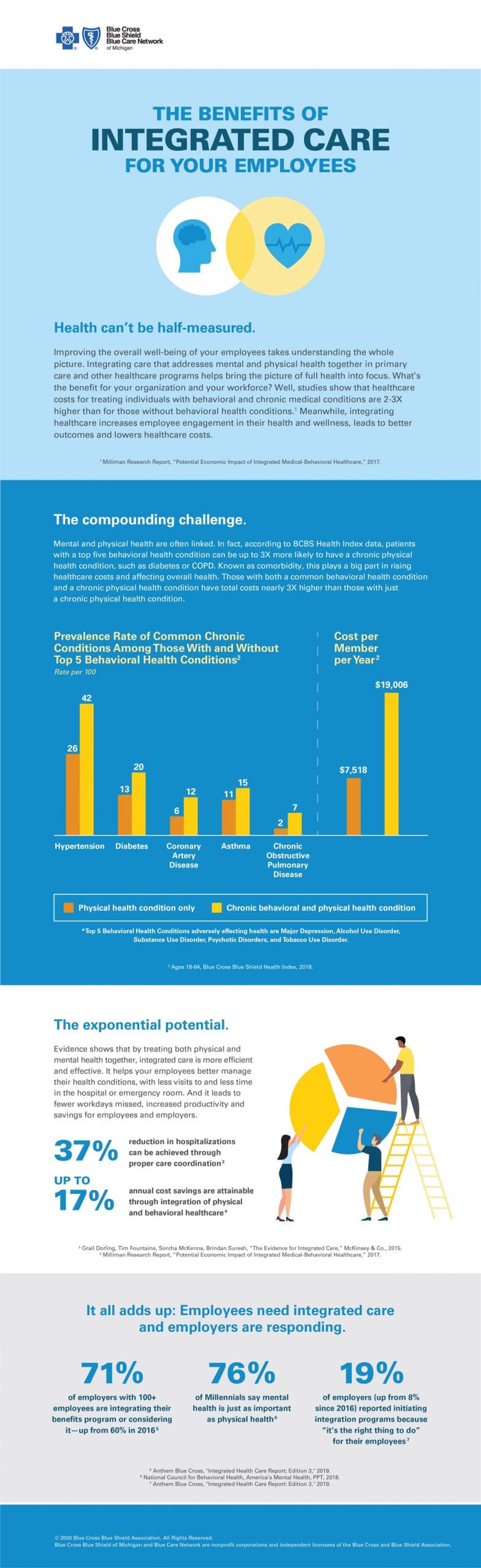
Simply put, comorbidity is the tendency of certain conditions to lead to other conditions. When behavioral and mental health conditions are not effectively treated, they can also impair self-care and adherence to medical and mental health treatments. As mentioned above, this is a major issue, and it comes at a cost. A critical piece in solving the comorbidity puzzle is proper coordination of care. This includes better supporting and empowering primary care providers (PCPs) to identify signs and have the resources to address behavioral and mental health and connecting them to behavioral health providers (BHPs). Digital platforms are helping this process and make it easier for health plans to share claims data and to provide predictive analytics. Treating behavioral and physical health together, and educating employees on healthy habits, can be more efficient and effective. In fact, research has shown that up to 17% annual savings are possible by integrating care.
INCLUDING SUPPORT BEYOND TRADITIONAL BENEFITS
Integrating care is about providing solutions for the whole person. That can extend even beyond the coordination of physical and mental health care to nontraditional wellness benefits like on-site access to dietitians, fresh fruits in the break room and access to sleep and resiliency apps. Programs can also extend into non-health benefits such as financial planning and coaching, tuition reimbursement and flexible work hours.
INTEGRATING CARE: THIS IS HOW
Treat the whole person.
Talk about and model health care solutions around the equal importance of physical and mental health. This means finding opportunities to embed mental health into wellness efforts, including chronic disease management programs for conditions like diabetes and asthma, which have high rates of comorbidity with depression and other mental health conditions.
Join networks that work together.
Choose health care networks that seamlessly connect primary care providers and behavioral health providers. When medical records, health information and resources are shared across providers, a whole picture of health comes into focus.
Connect the whole continuum.
Support health plan partners that empower primary care providers to collaborate with behavioral health providers. Tell your partner how important this is to your company and help to scale collaborative care models where you can — to make them accessible to your employees and their families.
Dr. William Beecroft, M.D., D.L.F.A.P.A., is a medical director of behavioral health at Blue Cross Blue Shield of Michigan. Dr. Amy McKenzie, M.D., is a medical director of provider engagement at Blue Cross Blue Shield of Michigan. More from MIBluesPerspectives.com:





