Disparities in Maternal Health Outcomes

Dr. Patricia Ferguson
| 4 min read
Dr. Patricia Ferguson, MD, is medical director at Senior Health Services, Emergent Holdings. Emergent Holdings is a separate entity contracted by Blue Cross Blue Shield of Michigan to perform administrative services for Blue Cross’ Medicare Advantage program. She is a fellow of the American College of Obstetricians and Gynecologists and is a member of the National Medical Association. She is a founder of the 501(c)3 nonprofit organization Each One Teach One.
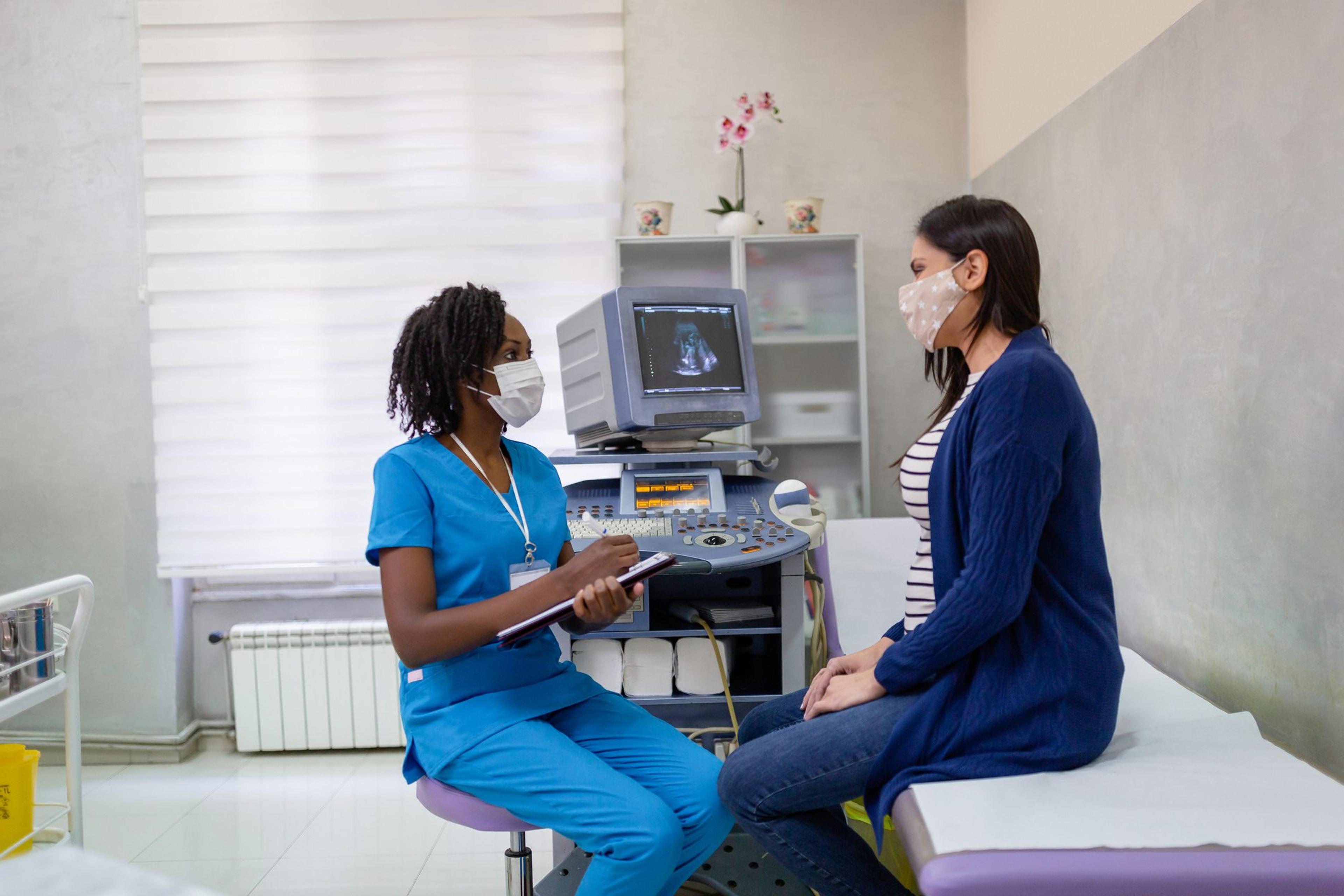
Women in predominantly Black communities have a 63% higher rate of severe maternal morbidity – unexpected outcomes from labor and delivery that impact a woman’s health, including death – than women in predominantly white communities. Women in predominantly Hispanic communities also have a 32% higher rate of severe maternal morbidity than women in predominantly white communities. These disparities in maternal health outcomes for individuals of color are a tragedy for families and many times, these deaths are preventable.
Social determinants of health
Social determinants of health have a significant influence on health outcomes for mothers and their children, including:
- Economic stability
- Neighborhood and physical environment
- Education
- Food security and access to healthy options
- Community and social context
- Access to competent, quality health care
Often, individuals who are struggling to make ends meet may have difficulty accessing the health care they need to maintain a healthy pregnancy. This could be due to lack of transportation to get to doctor’s visits or difficulty getting time off work to keep up with appointments, for example.
Unconscious bias
In addition to the effects of poverty on an individual’s life, too often racism and discrimination within society can further put people of color at risk for adverse health outcomes. Everyone carries unconscious biases that can affect how an individual’s concerns are viewed and responded to; even in a health care setting. For example, Black mothers may be more likely to have existing chronic conditions that put them at higher risk for complications after having a baby than white mothers, including anemia, hypertension, high body mass index and preeclampsia. But these risk factors are well-documented. Providers may not be asking their patients the right questions during their visits because they are making assumptions about them based on their own unconscious biases.
Schedule of doctor visits for pregnant women
Health care providers recommend a schedule of appointments for mothers during and after their pregnancies to ensure the baby is growing and the mother remains healthy. However, if there are complications or certain risk factors, providers may recommend more frequent visits. Here’s the traditional appointment schedule for mothers:
- Weeks four to 28 of pregnancy: One checkup each month
- Weeks 28 to 36 of pregnancy: Two checkups each month
- Weeks 36 to 41 of pregnancy: One checkup each week
- Six weeks after delivering baby: One checkup
There are urgent maternal warning signs that can occur during pregnancy or in the first year after delivery that should prompt an immediate trip to the doctor:
- Stopped or slowed fetal movement during pregnancy
- Thoughts of self-harm or harm to the baby
- Vaginal bleeding or leaking
- Vision changes
- Chest pain or rapid heartrate
- Difficulty breathing
- Dizziness or fainting
- Extreme swelling of face or hands
- Extreme tiredness
- Fever of 100.4 or higher
- Headache that won’t go away or gets worse
- Severe belly pain
- Severe nausea or vomiting
- Severe swelling, redness or pain in legs and arms
Schedule of doctor visits for babies
A separate schedule of appointments with a pediatrician is also recommended for babies following birth to ensure the first weeks and months of their lives are progressing appropriately and that any early warning signs of health issues are addressed quickly. Here’s the traditional well-child appointment schedule for infants during their first year:
- The first week (three to five days old)
- 1 month old
- 2 months old
- 4 months old
- 6 months old
- 9 months old
- 12 months old
Between ages one and two, toddlers are seen every three months by their doctor. They see the doctor again at age 2.5 and three, after which they see the doctor once a year. Encouraging and helping women who want to become pregnant, are pregnant or were recently pregnant to see their health care provider for regular well visits – as well as knowing the signs of urgent maternal health concerns – is a critical step in improving health outcomes for women of color and their families. Acknowledging unconscious bias in our systems and practices is another step to addressing its role in the decision-making process when providing care. Patricia Ferguson, M.D., is a physician consultant with Senior Health Services, Emergent Holdings. Emergent Holdings is a separate entity contracted by Blue Cross Blue Shield of Michigan to perform administrative services for Blue Cross’ Medicare Advantage program. For more health news and information, visit MIBluesPerspectives.com. Photo credit: Getty Images Continue reading:





