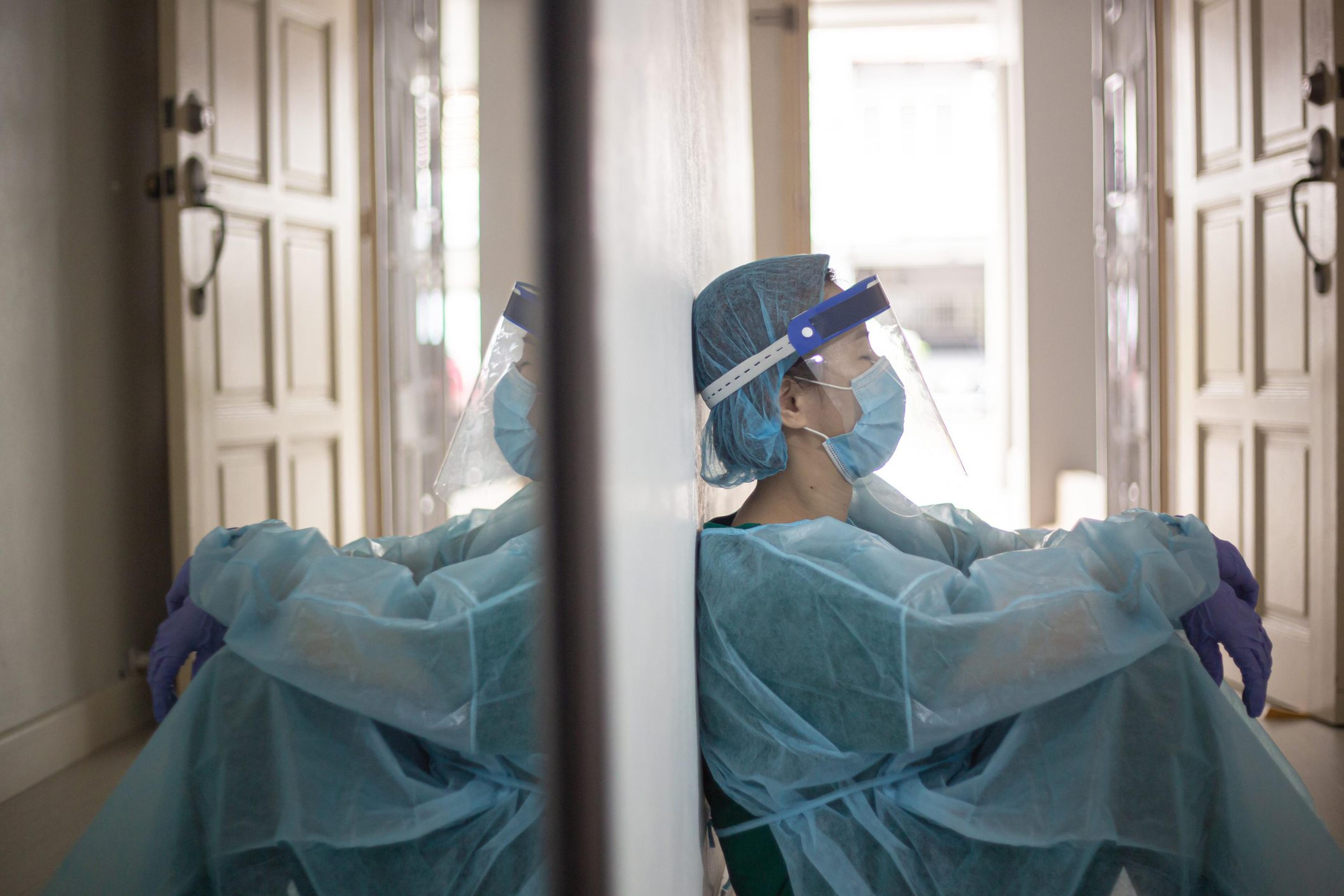
COVID-19 doesn’t just take an immense physical toll on the body. The mental and psychological effects felt by those who survived hospital stays and others who treated sick patients over the last two years is coming to light. A person’s psyche can be damaged when they witness or survive an extremely frightening and distressing event. This is known as psychological trauma. When psychological trauma disrupts the way a person functions for an extended period, posttraumatic stress disorder (PTSD) can develop. To be diagnosed with posttraumatic stress disorder (PTSD), psychological trauma must disrupt the way a person functions and interfere with their quality of life for at least one month. In some cases, PTSD symptoms persist for months and years. PTSD may coexist with other psychological problems, such as depression, anxiety, and substance abuse. Studies over the past year-plus have revealed symptoms of PTSD in both COVID-19 survivors and the healthcare workers who helped save their lives.
What are signs of PTSD?
Some signs and symptoms of PTSD can include, but aren’t limited to:
- Avoidance of activities that could trigger memories of a traumatic event. This could mean avoiding a friend or relative who may have witnessed the event or situation that has caused you so much trauma
- Experiencing event-triggered anxiety
- Irritability, angry outbursts, or aggressive behavior
- Issues with drug or alcohol use
- Reliving traumatizing experiences through flashbacks or nightmares
- Suffering from guilt, anger, anxiety, panic, depression, and inability to feel positive emotions
- Trouble sleeping and concentrating

How COVID-19 survivors and their families may struggle with PTSD
Studies have found that hospitalized patients who required a ventilator during the pandemic reported extensive symptoms of PTSD. Patients admitted to hospitals with COVID-19 experienced social isolation, physical discomfort, and fear for survival, factors that can all lead to an increased risk of developing PTSD. That risk isn’t just confined to COVID survivors, as multiple studies have found that family members of COVID-19 patients in intensive care may develop symptoms of anxiety, depression, and PTSD.
How healthcare workers may struggle with PTSD
The wellbeing and emotional resilience of doctors, nurses, and other healthcare workers have been tested at a unprecedented level during the COVID-19 pandemic. Healthcare workers have felt intense pressure to prevent severe illness and death related to COVID-19, often with a limited supply of medical resources. At the same time, they are regularly exposing themselves to the virus, creating new layers of anxiety that come with potentially bringing COVID-19 home with them and infecting family members. In 2021, a study was conducted to assess symptoms of depression, anxiety, and PTSD among public health workers in state, tribal, local, and territorial public health departments. Among 26,174 respondents, 32% reported symptoms of depression 30% reported symptoms of anxiety (30.3%) and 37% reported symptoms associated with PTSD. Other studies surveying healthcare workers and first responders have evoked reported thoughts of suicide or self-harm.
Coping with Stress, Anxiety and PTSD
There is no definitive cure for PTSD, but it is important for people to know that the condition can be effectively treated. Psychotherapy and medication are the most common forms of treatment. Cognitive processing therapy (CPT) is a trauma-focused, evidence-based psychotherapy treatment that is effective when delivered in-person or via telehealth. Exposure therapy is another method that can help COVID survivors confront their fears. Even those who were not hospitalized with a serious bout with COVID is being recommended more and more for people who are interested in but nervous about readjusting to everyday life in public after the pandemic. The following coping methods are specific to healthcare workers who may struggle with PTSD symptoms stemming from the pandemic:
- Seeking out social support
- Checking in with other colleagues; team cohesion can protect against the effects of traumatic experiences at work.
- Scheduling time of for gradual reintegration into society and personal life
- Preparing for worldview changes that may not be mirrored by others in one's life
Conversely, it is key for healthcare workers to lean on support systems to try and avoid these negative coping strategies:
- Use of alcohol, illicit drugs, or excessive amounts of prescription drugs
- Sudden big life changes
- Negative assessments and general self-deprecation relating to work contributions; Keeping too busy
- Viewing helping others as more important than self-care
- Keep work experiences bottled inside
If stress persists for longer than two to three weeks, individuals should consider reaching out to their primary care provider to decide if formal mental health treatment is a good option for them. Blue Cross Blue Shield of Michigan (BCBSM) offers behavioral and mental health resources, including those specific to the COVID-19 pandemic. Read more:
- Signs, Symptoms and Types of Hernias
- Why Should Employers Opt for Insurance Plans with an Integrated Health Savings Account Solution?
- The Benefits of Green Exercise
Photo credit: Getty Images





