RELEASE
What Blues members need to know about new autism coverage benefits
Sven Gustafson
| 3 min read

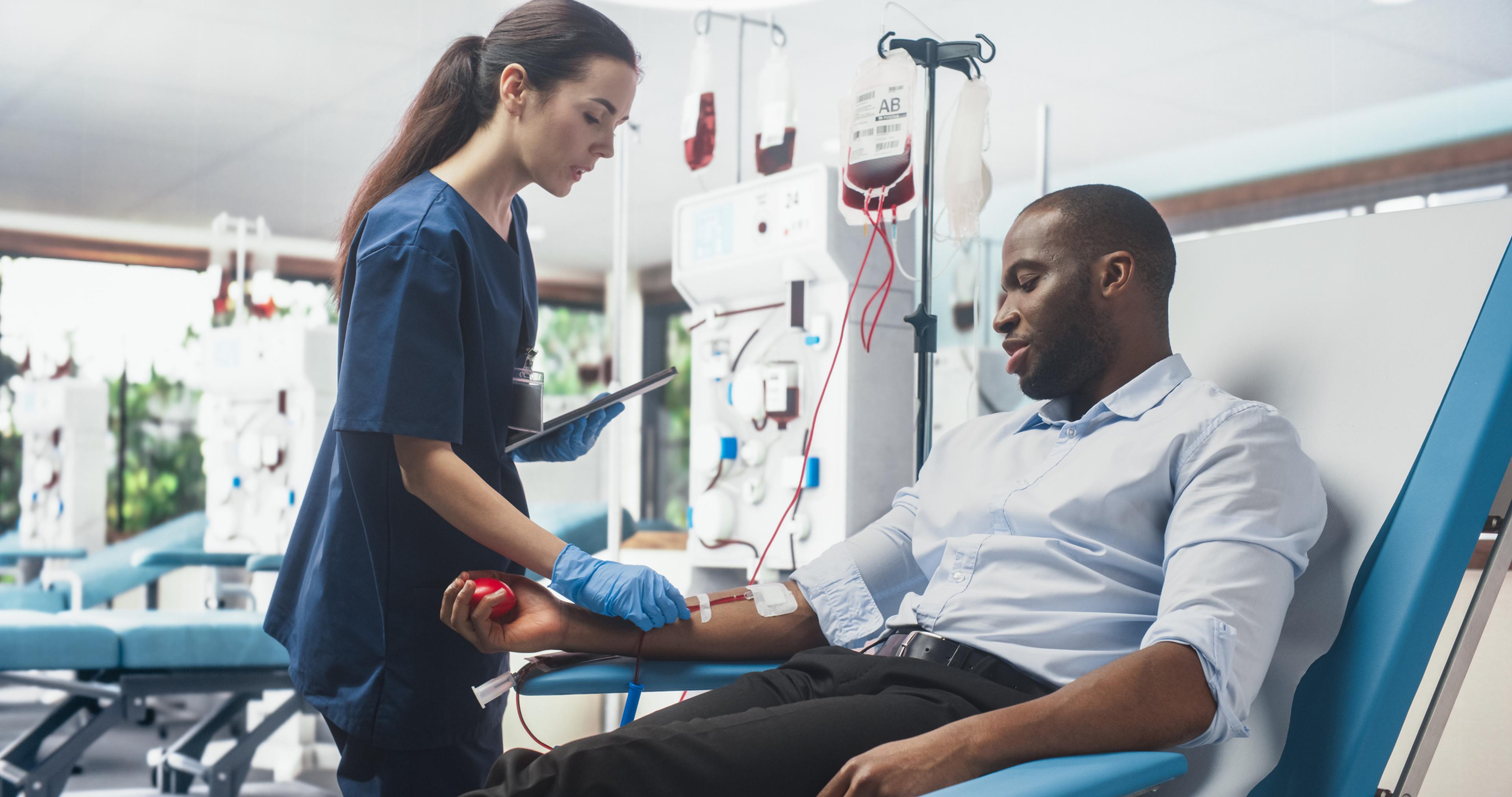
We’ve been getting a number of questions about new autism spectrum disorder benefits ever since a new law that expands autism benefits coverage in Michigan was signed in April. While we’re still working through many of the details, here’s what we can tell you.
What’s being covered, and when?
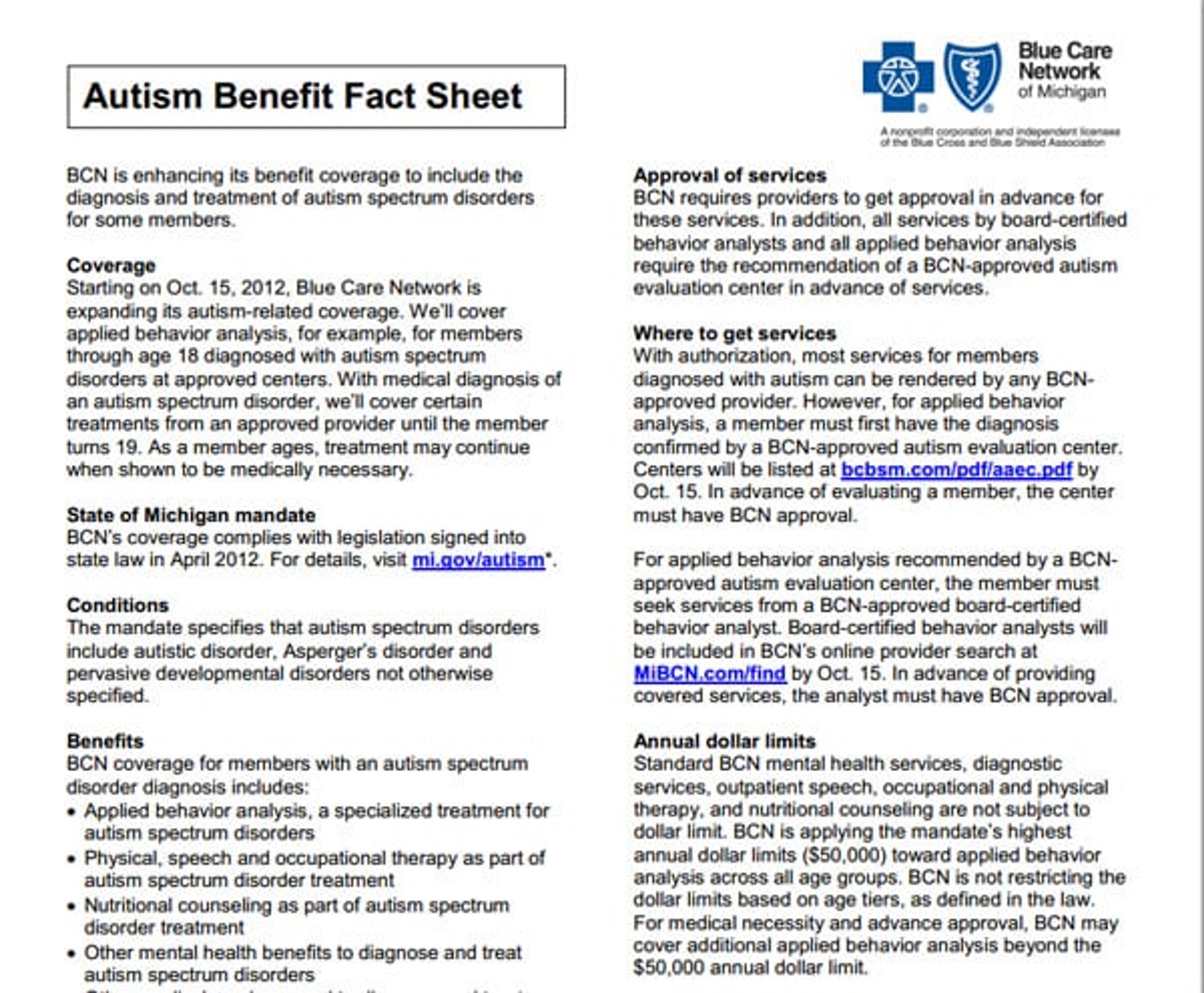
Both Blue Cross and Blue Care Network will expand their coverage for autism diagnosis and treatment beginning Oct. 15. We recognize this is an important health issue, and we believe we are the only health plan in Michigan that has offered Applied Behavior Analysis coverage options to group customers since 2009. Autism Spectrum Disorders that will be covered include autistic disorder, Asperger’s disorder and pervasive developmental disorder not otherwise specified. BCBSM and BCN coverage for ASD will include benefits for:
- Applied behavior analysis, a specialized treatment for ASD
- Physical therapy, speech therapy and occupational therapy as part of ASD treatment
- Nutritional counseling as part of ASD treatment
- Other mental health benefits to diagnose and treat autism
- Other medical services used to diagnose and treat autism
Do the benefits apply to all Blues plans?
Initially, the changes apply only to members of groups with underwritten health care coverage, meaning that either BCBSM or BCN assumes the risk for the cost of all covered services, and members with individual plans. Both BCBSM and BCN self-funded groups (where the employer assumes the risk), which aren’t subject to the new requirement, have the option to offer autism coverage beginning Jan. 1, 2013. Customer groups should call their sales manager for more information about the opt-in process. Not sure whether your group plan is underwritten? Contact your benefits administrator, or call the number on the back of your Blues ID card.
Will this make coverage policies more expensive?
Premium rates for members with group or individual coverage will not change as a result of the expanded autism benefits. The Blues will participate in a state-sponsored fund meant to reimburse insurers for ASD services provided in Michigan.
Are there dollar limits to the coverage?
Although the law defines dollar limits based along three age tiers, the Blues will apply the highest annual dollar limit of $50,000 across all age groups through age 18. Additional services require approval, and if they’re determined to be medically necessary, they’ll be paid.
What’s being done to help members who need ASD treatment?
To help ensure access to appropriate care, the Blues will designate approved autism evaluation centers that will make or confirm a diagnosis of ASD and also develop a treatment plan that would include a recommendation for ABA treatment, if appropriate. The Blues also will participate with Board Certified Behavior Analysts who will provide the applied behavior analysis services. Board-certified behavior analysts may also participate per claim for applied behavior analyst services. For information about facilities and specialists that can provide autism treatment services to members with a diagnosis of ASD, see our list of approved austism evaluation centers, or call the customer service number on the back of your Blues ID card.
What else do members need to know?
Depending on whether you have BCBSM or BCN coverage, it may be necessary to receive services only from participating network providers, obtain prior approval to have services covered, or meet other requirements. For more information, call the customer service number on the back of your Blues ID card. More information is also available through this fact sheet published at mibcn.com.