One in Four Michiganders Aren’t Getting Screened for Colon Cancer

Dr. James Grant
| 3 min read
James D. Grant, M.D. is senior vice president and ch...

More than one in four Michiganders are not getting screened for colon cancer, a statistic that crucially impacts another one: the stage at which colon cancer is diagnosed. According to data from the Michigan Department of Health and Human Services, from 2011 through 2018 in Michigan, more than half of colon cancer cases were first diagnosed in the late stage.
This is concerning because colon cancer is easier to treat, and good outcomes are more likely, when detected early. In fact, during colon cancer screenings, doctors often detect pre-cancerous polyps and remove them before they have a chance to develop into cancer. By comparison, in the late stage, colon cancer has spread to other parts of the body and is more difficult to treat.
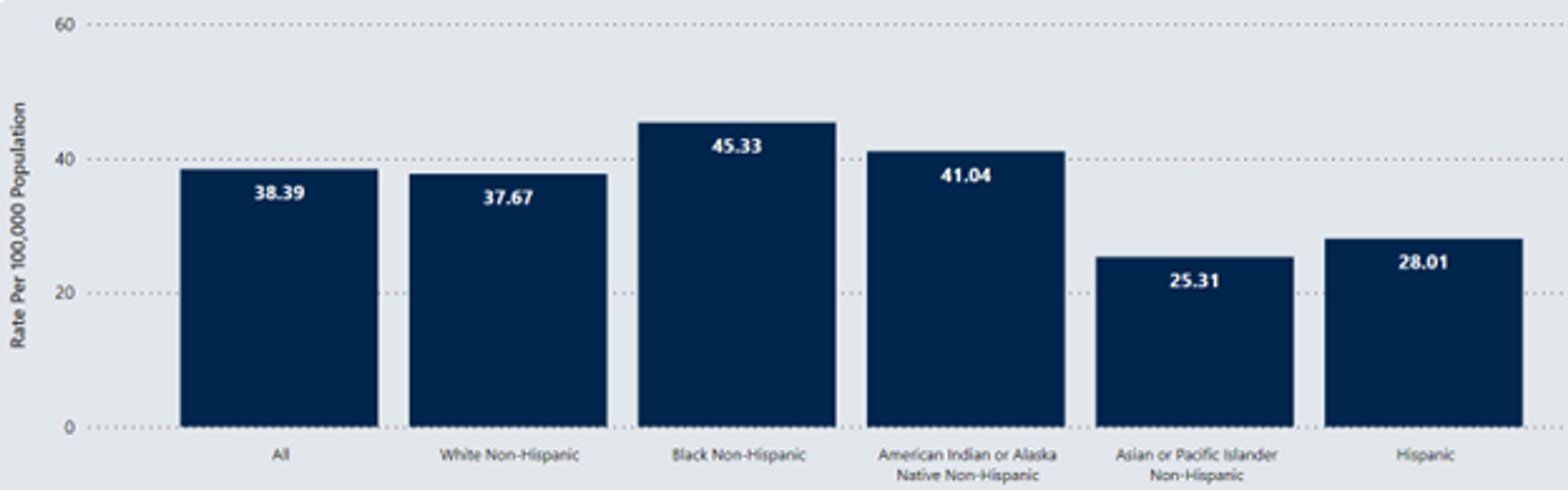
Between 2016 and 2020, roughly 26.5% of Michigan residents aged 50–75 did not have risk-appropriate colorectal cancer screenings performed. That number increases for certain racial and ethnic groups, as shown in the graph below.
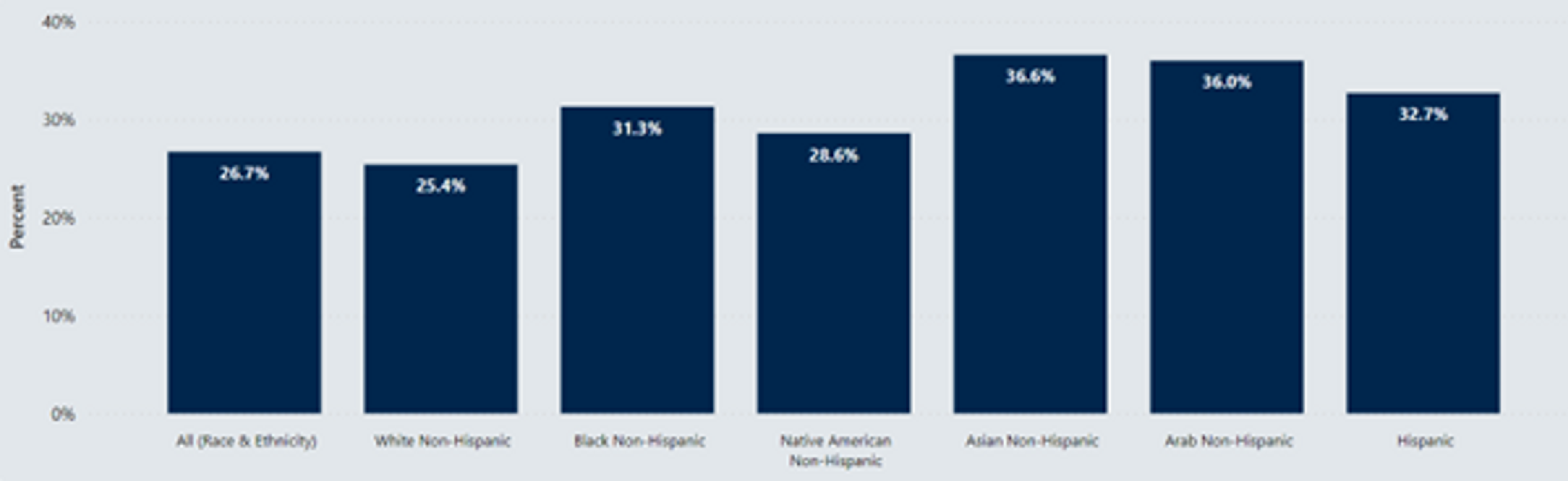
Racial disparities in colon cancer outcomes
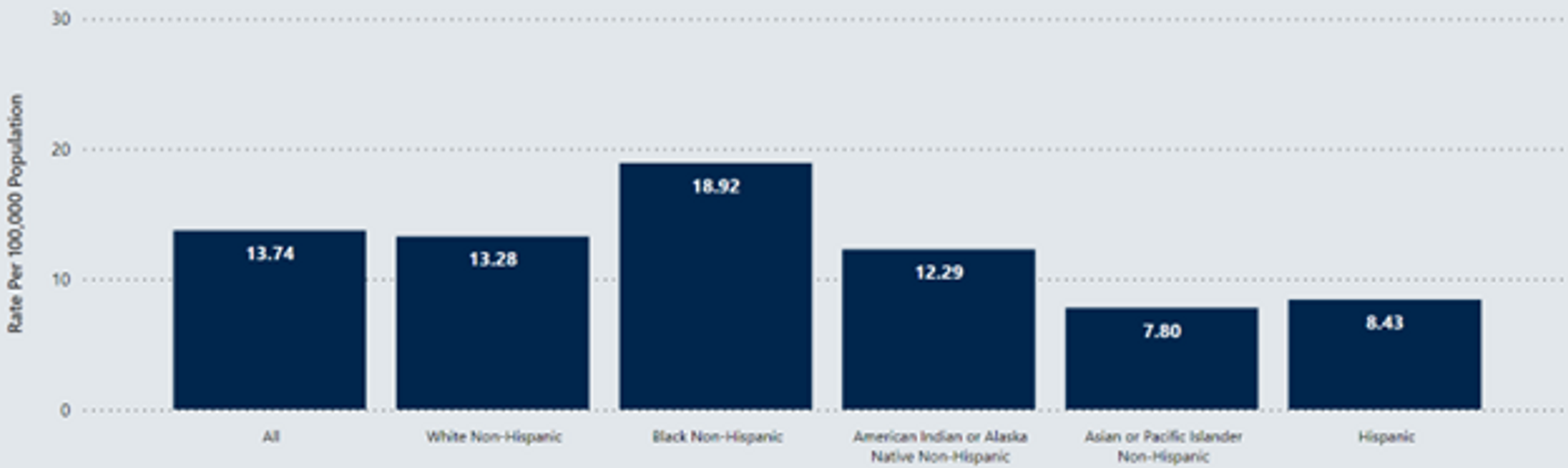
The need for appropriate colorectal cancer screening is particularly important when considering the racial disparity that exists in colon cancer outcomes for the African American population.
Nationally, African Americans have 20% higher incidence rates of colon cancer and 35% higher death rates from colon cancer. Similarly in Michigan, African Americans have roughly 18% higher incidence rates and 37% higher death rates from colon cancer.
The U.S. Preventive Services Task Force recommends adults between the ages of 45 and 75 and with no symptoms receive regular colorectal cancer screening. For most people, the gold standard of colorectal screening tests is a colonoscopy. For those with a health insurance plan that meets Affordable Care Act requirements, a screening colonoscopy is covered in full with no out-of-pocket expenses.
Individuals who have a family or personal history of colorectal cancer, polyps, inflammatory bowel disease or certain genetic disorders may need to begin screenings earlier than age 45. Individuals should talk with their doctor about when to begin colon cancer screenings.
Colon cancer prevention and screening
Some people may feel they do not need a colon cancer screening because they have no symptoms. However, people may have colon cancer and have no symptoms until the disease progresses to a more advanced stage. That’s why it is important to have regular screenings to identify a problem in its earliest, most treatable stage.
Individuals should check with their doctor if they are experiencing any of the following symptoms for more than a few days:
- A change in bowel habits, such as constipation, diarrhea, or narrow stool
- Rectal bleeding with bright red blood
- Dark brown or black stool, which could indicate blood in the stool
- Abdominal cramping
- Losing weight without trying
- Feeling the need for a bowel movement that doesn’t go away after having one
- Fatigue or weakness
Individuals should talk with their doctor about their symptoms and health history, and to come up with a plan for colon cancer screening.
Blue Cross Blue Shield of Michigan and Blue Care Network cover colorectal screenings for most members beginning at age 45 to align with the recommendation of the U.S. Preventive Services Task Force. For more information, click here.
James D. Grant, M.D., is senior vice president and chief medical officer at Blue Cross Blue Shield of Michigan.
Photo credit: Getty Images