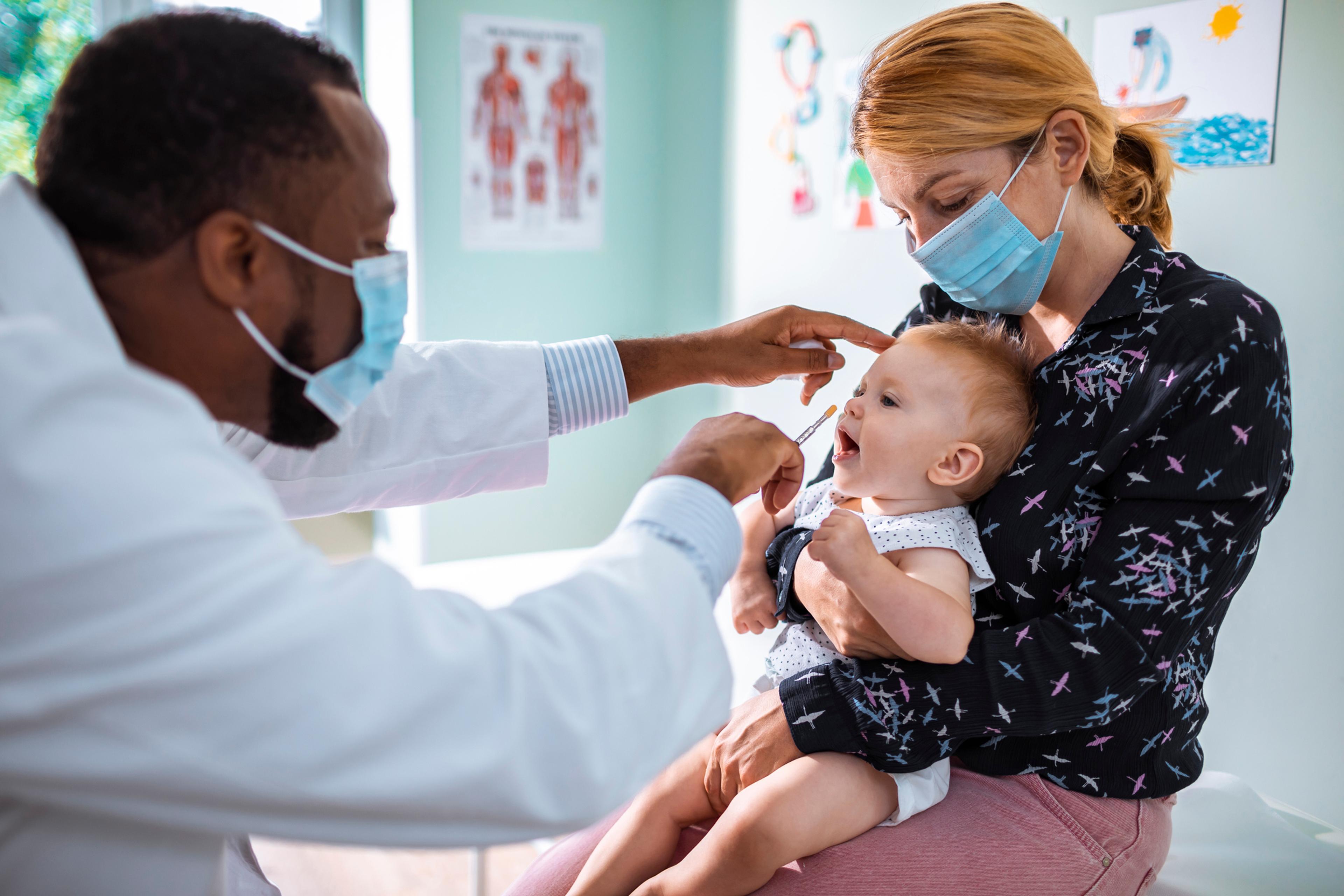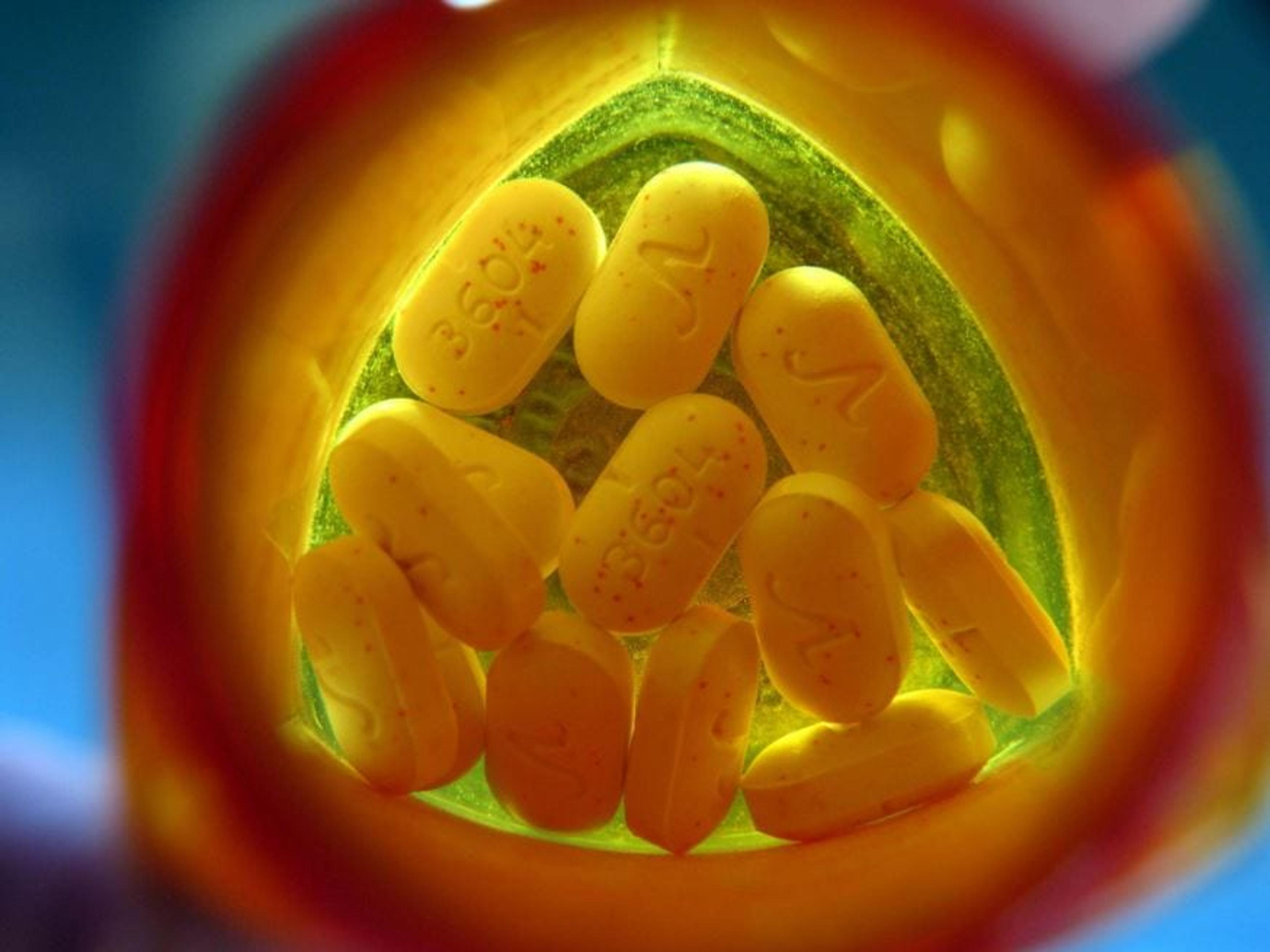
Opioid abuse and overdose has become a nationwide epidemic. According to the Centers for Disease Control and Prevention, 91 Americans die each day as a result of an opioid overdose. In addition, more than six out of 10 drug overdose deaths involve an opioid of some sort. But there is still a lot of confusion about what opioids are, why they are so addictive, and how something prescribed by a doctor can be so deadly. Because this epidemic is so far-reaching, here is what you need to know about opioids: What is an Opioid? “Opioids are strong pain relieving drugs often prescribed for moderate and severe pain associated with surgeries or injuries,” says Jody Gembarski, a clinical pharmacist with Blue Cross Blue Shield of Michigan. You’re likely familiar with the most commonly-used prescription opioids: hydrocodone (Vicodin®), oxycodone (OxyContin®), morphine and fentanyl. The illegal drug heroin is also an opioid but has no medical use. Prescription opioids are effective in relieving pain but come with serious risk, that’s why all opioids require a prescription by a licensed health care provider. “They should be used for the shortest possible duration when other non-opioid treatments are ineffective, not as a consistent way to treat chronic pain unrelated to a cancer diagnosis or end-of-life care,“ says Gembarski. Why Are They So Dangerous? “Anyone taking an opioid runs the serious risk of developing addiction,” Gembarski says. “When patients take opioids in higher doses or more frequently than prescribed, or for a reason other than pain relief, they become dangerous,” she says. Abuse of prescription opioids can even lead to heroin use. “Opioids have the ability to alter the brain’s chemistry,” she says. “Over time, they can cause the body to stop making endorphins on its own, and endorphins are what make us feel good. When we can’t make endorphins ourselves addiction develops and patients compulsively seek out these drugs.” While this is reversible, it can take a long time for the brain to function normally again. There’s also a concern for accidental overdose and death with opioids. Taking too many opioids or when combining them with other medications that cause sleepiness, such as muscle relaxants, sleep aids or benzodiazepines (such as diazepam or alprazolam), your breathing can be slowed or you can even stop breathing altogether. What Should You Know Before You Start Taking Them? Many people have the misconception that opioids are meant to stop pain altogether. “You may still have some level of pain, just at a more manageable level,” Gembarski says. She stresses the importance of open communication between you and your doctor to determine whether the medication is even necessary and give insight into how to manage its effects. “Patients should always ask their doctor if the prescription opioid is right for them in their given situation as there are many non-opioid alternatives for pain management,” Gembarski says. “If your doctor prescribes an opioid it is also important to have your doctor explain what you can expect as a result of use,” she says. Don’t assume your doctor will know for certain how long you will be using the medication. “Everyone experiences pain differently and doctors can’t anticipate how long you will need to take them,” Gembarski says. “It’s also vital to inform your doctor about other medications you’re currently taking, both prescription and over-the-counter,” she says. “There could be drug interactions that can lead to serious side effects and consequences.” Education is key when it comes to the safe use of opioids and avoiding the effects of abuse and addiction. Visit these other blogs for more information: