New Guidelines Help Doctors Plan for Safe Surgery After a Patient’s COVID Infection

Dr. James Grant
| 2 min read
James D. Grant, M.D. is senior vice president and chief medical officer at Blue Cross Blue Shield of Michigan. Dr. Grant is a native Michiganian and graduate of Wayne State University School of Medicine. He completed his post graduate training at Northwestern University Medical Center in Chicago. He is a diplomate of the American Board of Anesthesiology, completed his recertification in 2008 and is an associate examiner for the Board.
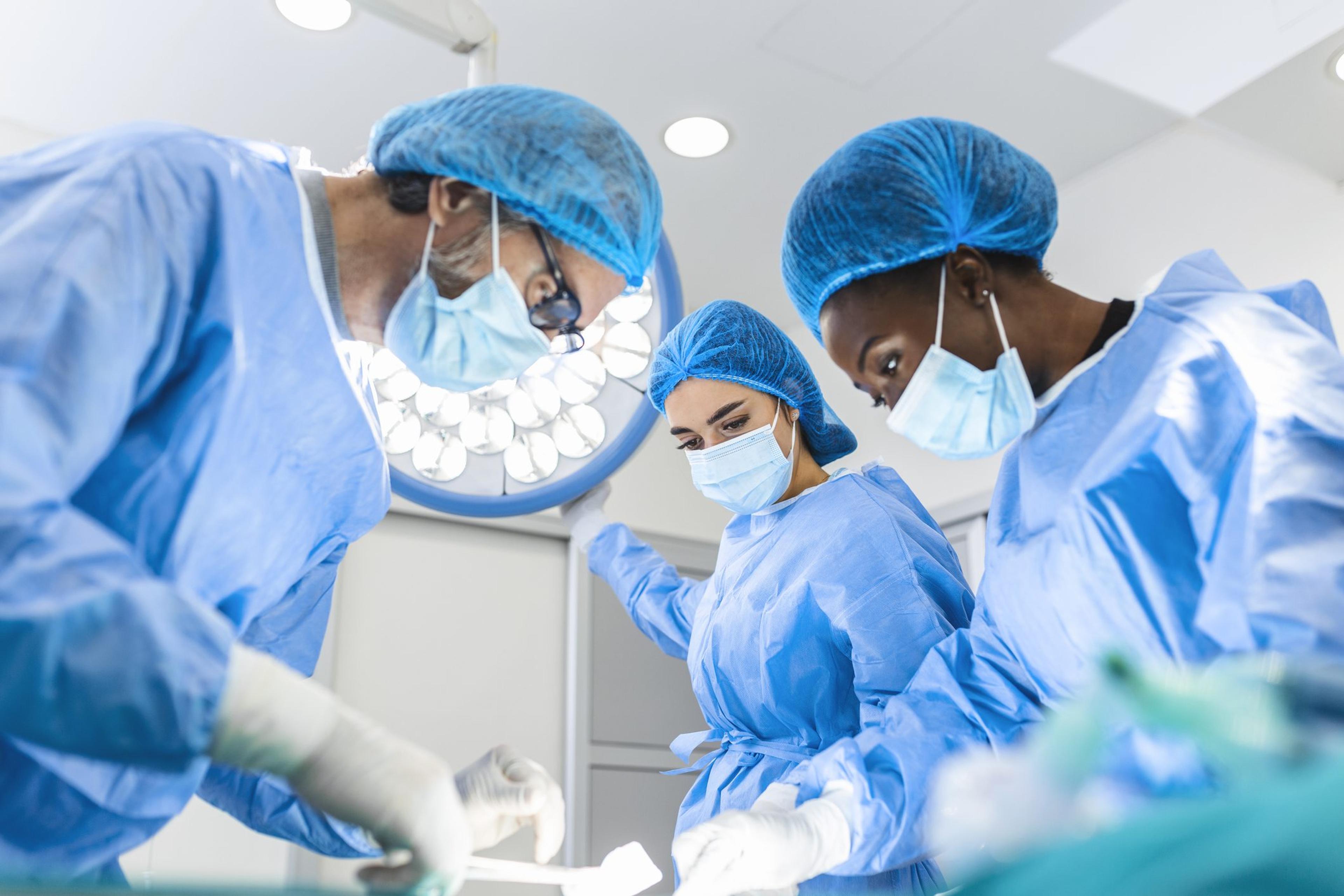
How soon after having a COVID infection is it safe for you to undergo a surgical procedure? Surgeons and anesthesiologists have pondered this question since the beginning of the COVID pandemic. This issue hits home for me, as a practicing anesthesiologist who has participated in thousands of surgeries. Because COVID is predominately a respiratory illness, doctors want to make sure your lungs are healthy enough to withstand the demands of anesthesia and post-surgical recovery. This is because surgery using general anesthesia places some demands on your body. General anesthesia slows down your body’s functions while it keeps you from feeling pain. This affects your body’s breathing and blood flow. Research suggests that a moderate or serious COVID illness can affect a patient’s recovery after a surgical procedure and can put a patient at higher risk for post-surgical complications. Recently, the American Society of Anesthesiologists and the Anesthesia Patient Safety Foundation issued a set of recommendations that help doctors evaluate and determine when a COVID-infected patient can safely undergo elective (non-emergent) surgery. When planning for a safe procedure, the guidelines recommend your surgical team evaluate you and consider:
- The severity of prior COVID infections
- The potential risk of any ongoing symptoms
- Your overall health status
- Any additional conditions, such as heart disease, asthma, or diabetes
- The complexity of the surgery
The guidelines also indicate that those who are vaccinated can safely undergo surgery when they have no COVID symptoms and are no longer infectious. Evidence indicates that surgical risk is less in vaccinated patients who get COVID. For those who are unvaccinated, the recommendation is to wait seven weeks after COVID infection and ensure there are no lingering COVID symptoms at the time of surgery. These recommendations guide physicians in determining the best time for your surgical procedure, if you have had COVID. Clinical guidelines such as these are helpful as we adjust to the continued presence of the COVID virus in our daily lives. If you have any questions or concerns, please talk with your surgical team. James D. Grant, M.D., is chief medical officer at Blue Cross Blue Shield of Michigan. More from MIBluesPerspectives:
- Exercise After COVID: Michigan Runner Races Again After ‘Severe’ Bout with Virus
- Living with Headaches from Long COVID
- Blue Cross Helps Customers and Members Through Pandemic
Photo credit: Getty Images