Tools to Build Your Confidence

Blues Perspectives
| 3 min read

At Blue Cross Blue Shield of Michigan, we’re constantly investing in and adapting to the latest digital technologies. Our Member Channels and Applications IT Team creates the self-service tools to help each of our members get the most out of their plans. “Our role is to create and support a simple, seamless, digital ecosystem across the health care community by leveraging personalized insights and tools,” says Ketan Joshi, Director of Channel Apps and Tools. All 5 million-plus Blue Cross members have access to our innovative technologies, from voice recognition to data-driven integration. These tools help guide them with information on their plan, benefits and coverage to make the best decisions for their health. Here are some of the ways we enhance the experience for Blue Cross members through our digital tools:
Member Portal
It all goes through the portal.
Our Member Portal is the home base for a member’s plan information and questions. Members can log in and check their claims, view benefits and balances, or search for providers and care centers. The Member Portal also helps members manage health and wellness programs like WebMD or the BWell health program to educate themselves on different conditions and treatments and stay on top of their day-to-day health activities. Blue Cross Blue Shield of Michigan’s Member Portal includes a variety of tools such as:
Mobile App
Go from screen time to getting screened.
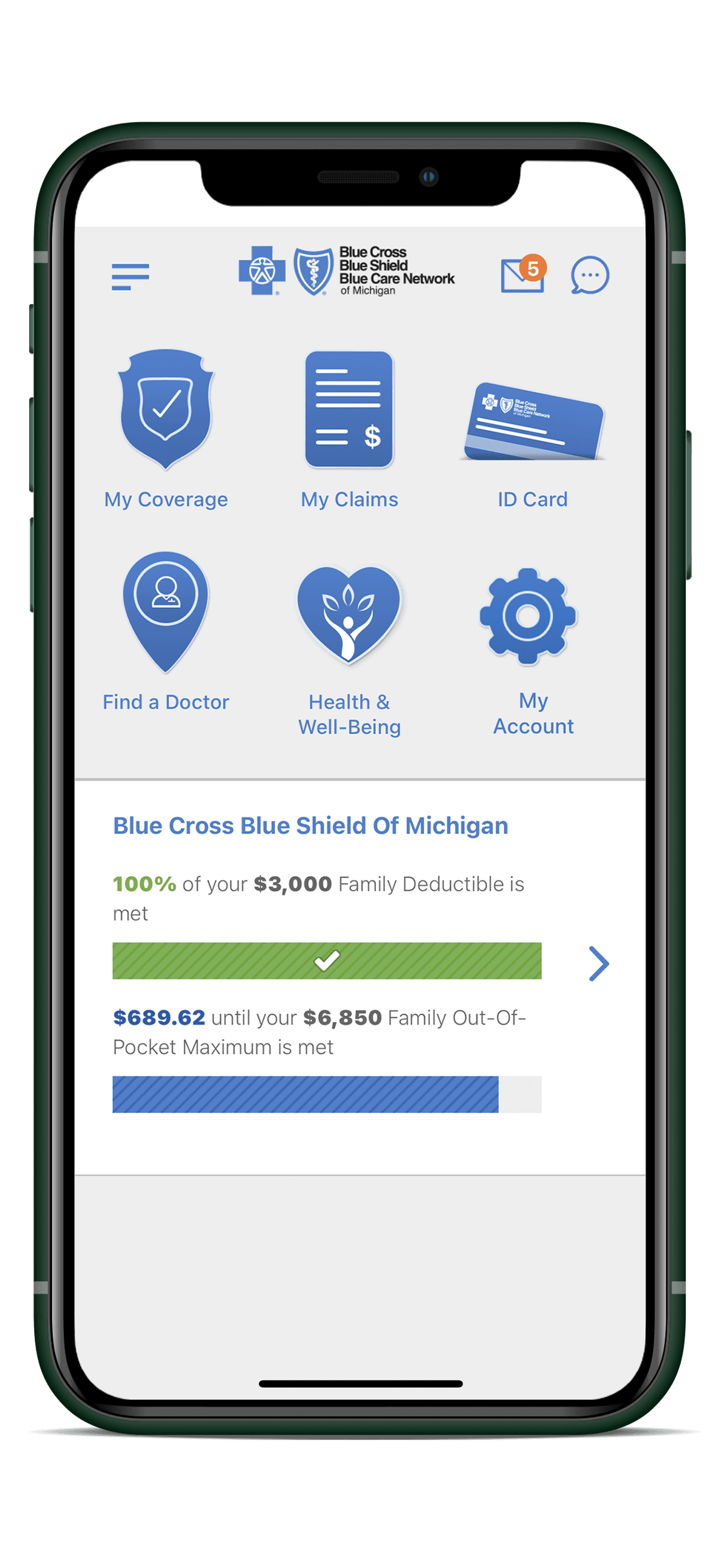
Our Mobile App provides you everything the Member Portal does, but right at your fingertips, anytime, anywhere.
Smartbot
This is the one place we welcome bots.
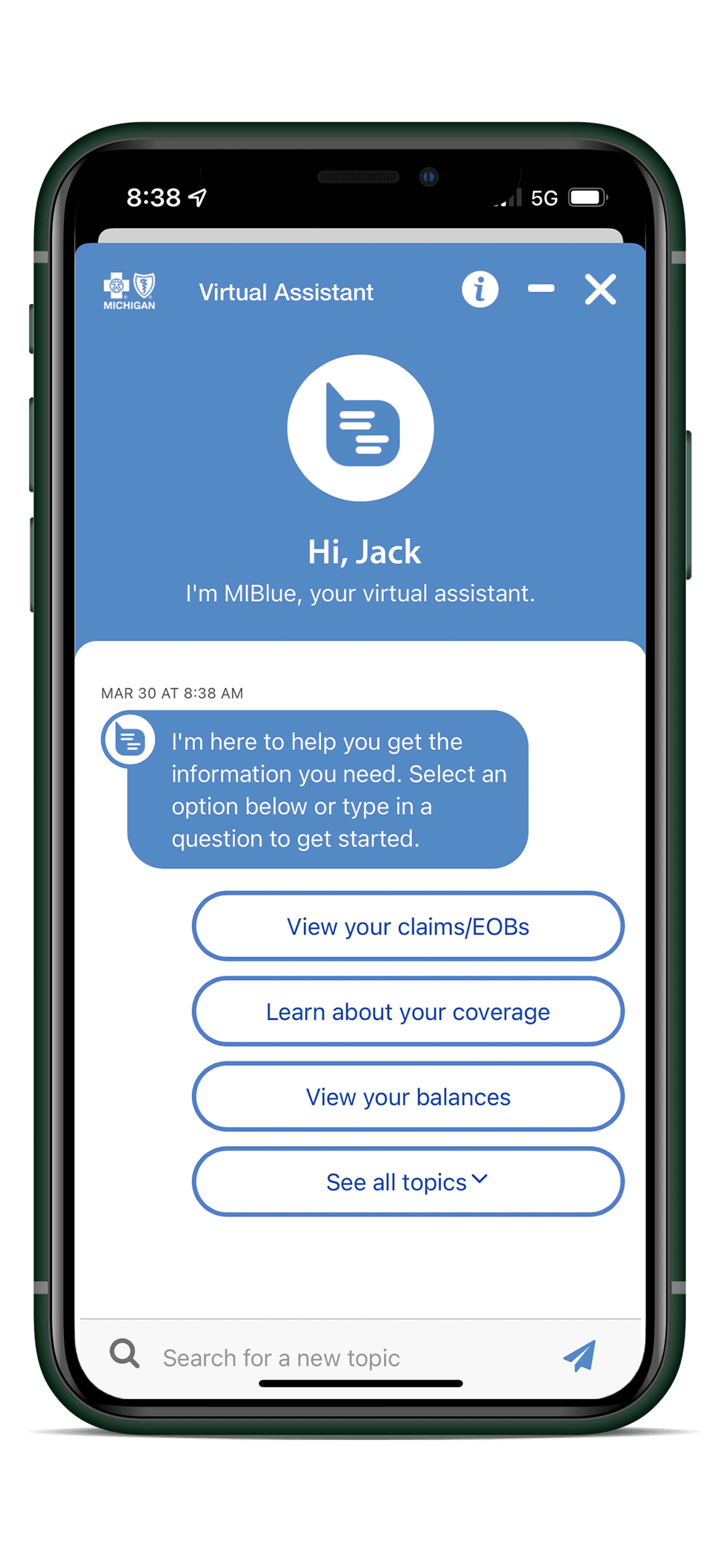
Using Artificial Intelligence (AI), we created a Smartbot to integrate content and pull out the intelligence it has already acquired to make each user experience as efficient and seamless as possible.
Search
Search with a purpose.
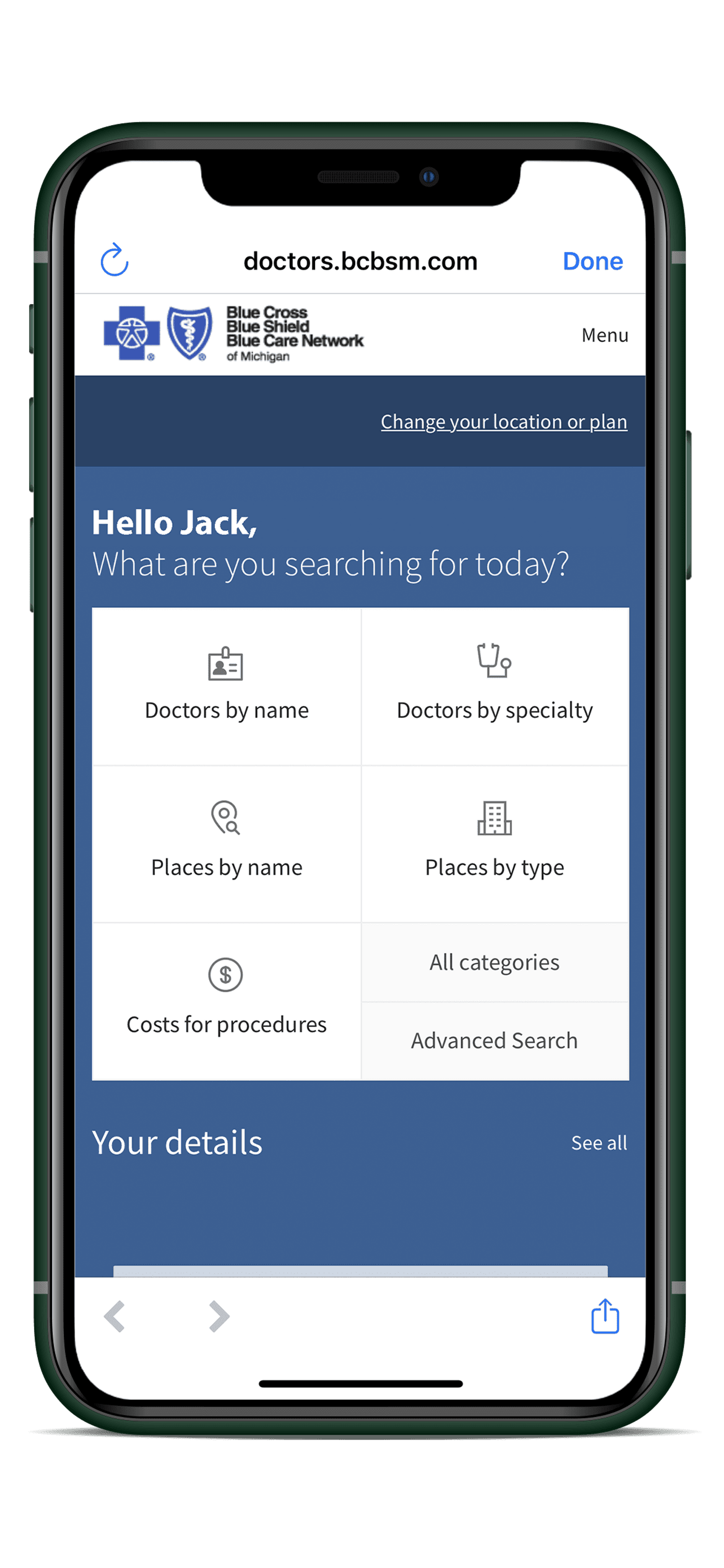
Our search tools allow members to explore lists of providers and treatment costs, find specifics on coverage and costs under their plan, or review filed claims and bills. This search technology leverages online tools and Smartbot insights to keep track of claims, upcoming appointments, and other health care provider interactions.
AI.ME
Intelligence customized for you.
With our AI.ME technology, members can move away from the Smartbot and transfer all their information into the cloud. This allows members to scan claims and use artificial intelligence to alert them on upcoming appointments, making for easier decisions based on their health and specific Blue Cross coverage.
Bringing all these tools to life and ensuring they function efficiently for the member is no small feat. “Everything that goes on behind the scenes to actually run the business operations is leveraged in real-time for the member,” says Joshi. His team uses more than 20 technologies connected at over 250 integration points to link various subsystems and third-party applications. Bringing all that information together in one place to make it accessible and functional for our members is like weaving a tapestry of information, creating a unique health care image for each individual. The tools Joshi and his team builds are crucial in pushing innovation and improvements to our members’ overall health care and membership experience. More from MIBluesPerspectives:
- From Driving Innovation to Award-Winning Recognition
- The Role of Artificial Intelligence in Health Care
- New Technology, Data Practices Aim for Improved Health Outcomes, Reduced Costs
Photo credit: Getty Images