Debunking Sickle Cell Disease Myths and Misconceptions

Dr. Gina Lynem-Walker
| 3 min read
Dr. Gina Lynem-Walker, MD, is a quality medical dire...

Myths and misconceptions about the blood disorder known as sickle cell disease extend globally. They can lead to racial and sociodemographic stereotypes, biases in health care settings, negative attitudes toward patients, and mental health problems for the patients already dealing with a devastating physical condition.
Debunking these myths can soften the stigma around sickle cell disease and help individuals understand it better. Here are some common misconceptions.
Myth: Only Black people suffer from sickle cell disease.
Fact: While it’s true that sickle cell disease is most prevalent among Black people, people of any ethnic background can inherit it. According to the U.S. Centers for Disease Control and Prevention (CDC), one out of every 16,300 Hispanic-American births are affected by sickle cell disease. People of Indian, Asian, Middle Eastern and Mediterranean heritage are also particularly prone to the disease, which occurs more often among people from parts of the world where malaria used to be or still is common.
About one in every 13 Black or African American babies are born with the sickle cell trait. Nearly one in every 365 Black births are affected by sickle cell disease, according to the CDC.
Myth: Sickle cell disease is a contagious blood-borne disease.
Fact: Sickle cell disease is a genetically inherited disease that is present at birth. Both parents must carry the sickle cell trait for a child to inherit sickle cell disease. It’s not a disease that can be contracted later in life; you are either born with it or you will not be diagnosed with it, even if exposed to the blood of someone who has the disease or carries the sickle cell trait.
Myth: People with sickle cell disease are “lazy.”
Fact: Sickle cell disease is often an invisible disease, but one of its most common symptoms is extreme fatigue, especially among people suffering from sickle cell anemia. Sickle cell anemia can also cause sudden, intense bouts of pain – called vaso-inclusive crisis – that can only be eased with opioid painkillers.
This myth of “laziness” is a dangerous one because it can lead to false impressions in schools and workplaces about the person living with sickle cell disease.
Inclusive, understanding and supportive work and school environments are crucial in that they can help people with sickle cell disease perform to the best of their ability without being discriminated against.
Myth: A baby born with sickle cell disease is doomed to live a short life.
Fact: Decades ago, it was more common for children born with sickle cell disease to die before adulthood. But according to the CDC, more than 95% of American newborns with sickle cell disease will live to be adults. Every newborn in the U.S. is screened for sickle cell disease. Early diagnosis allows doctors to treat and prevent infections and stroke, which were major risk factors for high mortality rates in children with sickle cell disease years ago.
Living with sickle cell disease
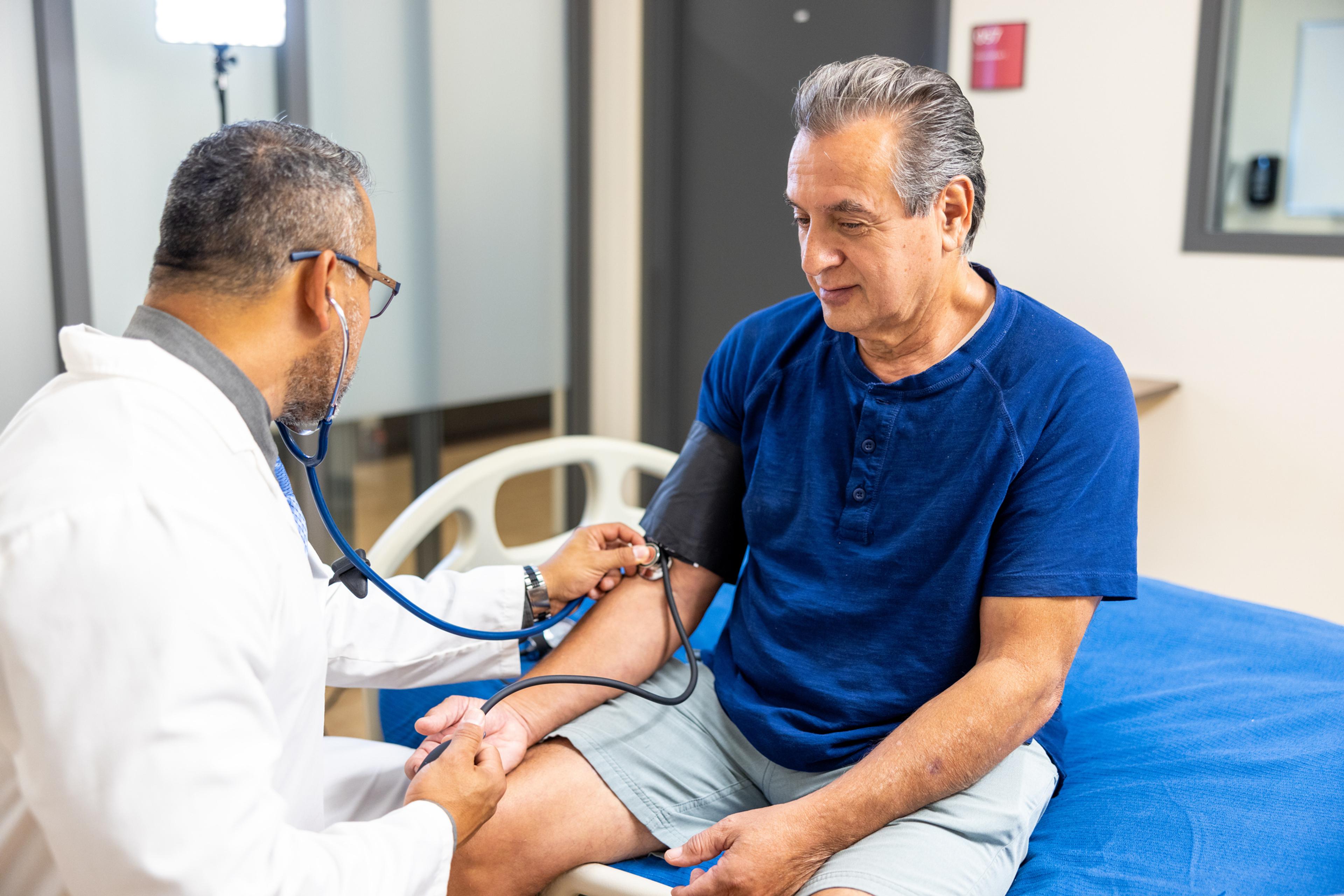
Sickle cell disease can be a painful condition that carries other complications and increased risk factors for other diseases. Managing sickle cell disease takes prevention strategies, including:
- Attending regular checkups with a primary care provider
- Following treatments prescribed by a provider, including taking medication as directed
- Preventing infections by regularly washing hands
- Practicing healthy habits like drinking eight to 10 glasses of water per day and eating nutrient-rich, non-processed foods
Gina Lynem-Walker, M.D., is an associate medical director at Blue Cross Blue Shield of Michigan. For more health news and information, visit MIBluesPerspectives.com.
Click here for BCBSM's Sickle Cell Disease Toolkit:
Photo credit: Getty Images
Keep reading: