‘It’s My Duty’: How Doctors are Working to Reduce Health Disparities Among Black Patients
Amy Barczy
| 7 min read
Amy Barczy is a former brand journalist who authored...

Dr. Cheryl Gibson Fountain, MD, FACOG, is highly regarded in her field as an obstetrician: her achievements include the first African American female president of the Michigan State Medical Society and serving as the representative from the American College of Obstetricians and Gynecologists to the American Medical Association.
Yet last year, as she was helping her late father with his health issues and standing alongside her pregnant daughter as she navigated complications – she felt her skin color was speaking louder than her credentials. Doctors dismissed her concerns as a patient advocate – and the concerns of her family members.
“When you go into a health care system – you should be able to be a patient like everyone else, regardless of your race,” Gibson Fountain said.
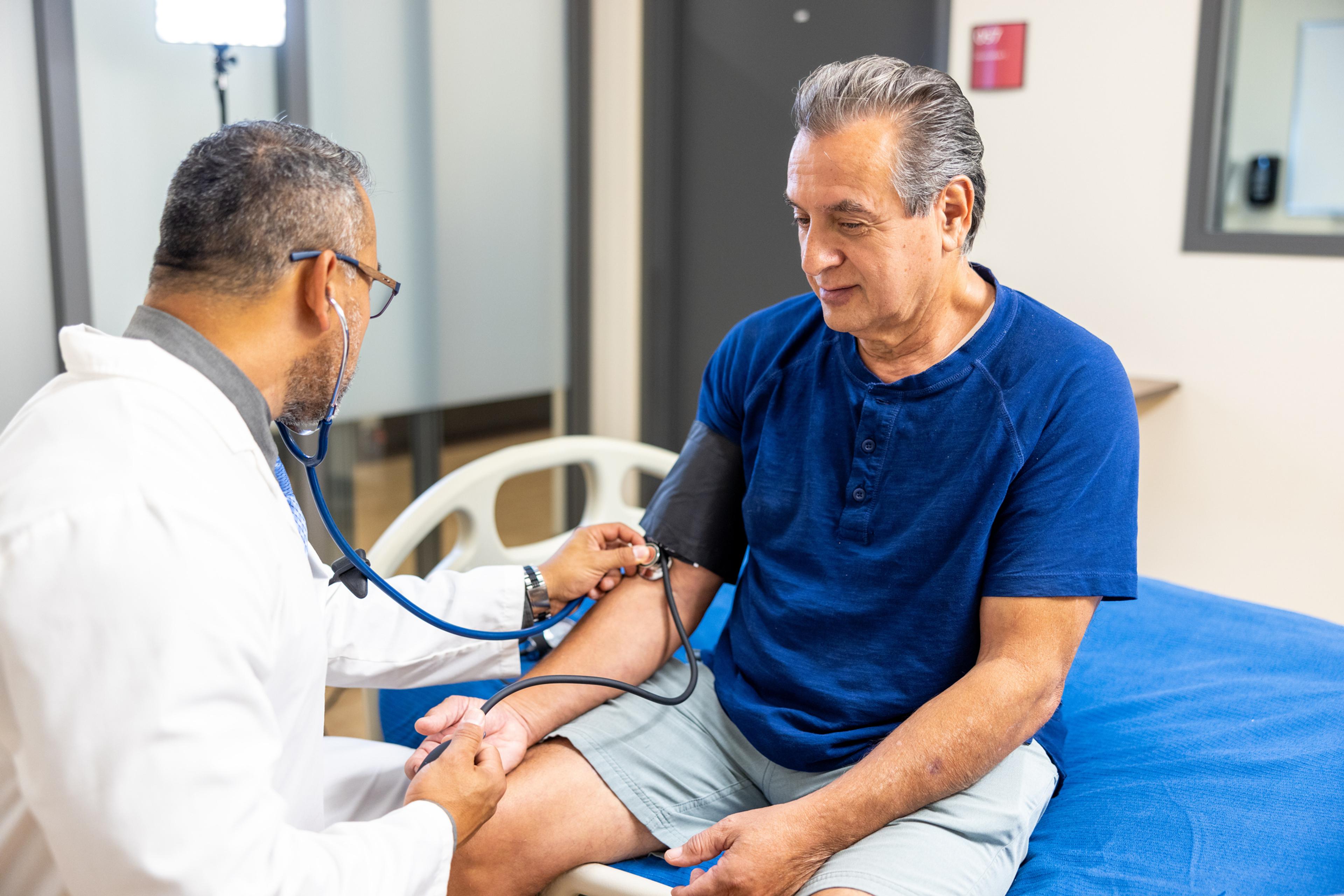
Patients from minority backgrounds are often at risk of worse health outcomes than their white counterparts: they have lower life expectancies, and often have higher rates of chronic conditions like diabetes and heart disease.
One of the most glaring examples is maternal mortality: death rates continue to increase among Black women who are pregnant or recently gave birth in the U.S. Yet many of these deaths are from conditions like high blood pressure and postpartum hemorrhage that have interventions available.
The causes are systemic – social determinants of health like education, health literacy, income and environment all play a role – as well as longstanding issues of racial biases and prejudices in medicine. It takes dedicated providers working diligently to overcome decades of wrongful practices and harmful policies, and to teach the next generation of doctors to do better for all patients.
On the front lines
Among the ranks of doctors working to improve the field is Dr. Gibson Fountain, who is a medical director at Blue Cross Blue Shield of Michigan.
Gibson Fountain guides best practices for health care institutions across the country and as a part of the statewide Blue Cross Physician Diversity Council.

Also on the council is Dr. Patricia Wilkerson-Uddyback, MD, MBA, FACEP, who works in emergency medicine in Detroit.
“I am so blessed to be able to practice medicine. As an African American woman practicing in a predominantly African American community, I feel it’s my duty to be a resource to my patients,” Wilkerson-Uddyback said. “I have lived in Detroit my whole life. I am very committed to the citizens of this community. I am very committed to do the best I can with what I have.”
In Detroit, many Black patients Wilkerson-Uddyback sees are still feeling the impacts of the pandemic: they don’t want to go to the doctor’s office and get COVID. They are also afraid of the cost of care.
It means sicker and sicker patients are showing up at the emergency room.
“There is no question in the last three years, the patients I serve – Black Americans – are much sicker now than they were before,” Wilkerson-Uddyback said. “They are waiting to come in.”
Waiting to see a doctor has dire effects for any patient. In the primarily Black population Wilkerson-Uddyback serves in Detroit, she sees the impact firsthand. Many providers retired during the pandemic; and many patients aren’t taking their medications as prescribed – as they have run out of pills, or are rationing pills to save money, or sharing them with a loved one without insurance. At home, there are gaps in the support systems from COVID pandemic deaths.
“Patients are going to be in the hospital much longer to deal with all of the issues. Their overall health is going to be much worse: even if we help them to the point that they can be discharged, their bodies take a toll,” Wilkerson-Uddyback said. “Patients are going to have higher health care costs. The care we provide isn’t free – in most situations, there’s a deductible or out of pocket costs – that’s what’s deterring patients from seeking out care. They look at me and they say, ‘I can’t afford this.’ But waiting doesn’t help you avoid the problem.”
Addressing social determinants of health – like increasing access to transportation, healthy foods and health care literacy – is critical to helping people improve their quality of life. Wilkerson-Uddyback sees education as the biggest opportunity for Black Detroiters.
“The number one social determinant of health that we can really focus is to ensure every student graduates from high school,” Wilkerson-Uddyback said. “That’s going to mean better employment, which means better health benefits. Better income also means living in a better environment.”
Teaching empathy
To Gibson Fountain, biases are preventing providers from providing empathetic care to all their patients.
“How do you train someone to be empathetic?” Gibson Fountain said. “Believe Black people when they’re talking to you. We’ve got to do something about addressing the racism and unconscious bias. There are a whole host of people that are mistreated.”
Wilkerson-Uddyback said she helps show resident doctors she works with how to provide culturally competent care.

“My patients are like family in many ways; I understand them – that brings another level of care that you just can’t buy,” Wilkerson-Uddyback said. “I can pass that on to my residents and medical students I work with.”
Building empathy starts by asking questions beyond “how are you feeling?” and “how long did you have the fever?” said Wilkerson-Uddyback. It means asking what is going to happen once they leave the hospital: who is going to take care of them? Can they afford the medications that are being prescribed? Do they have a doctor to follow up with?
“These questions can help make an impact, so they don’t keep coming back to the ER. It’s about asking the hard questions, and not assuming they’re not taking their medication because they don’t care,” Wilkerson-Uddyback said. “As providers we need to continue to educate ourselves about the variables that impact our patient’s health – not just the science that we learned in medical school. We need to really be in tune with the dynamics that happen when they’re at home and be open to understanding the cultural space.”
Overcoming institutionalized racism
The experience of being Black in the health care system has come a long way. As a teen in high school, Dr. Gibson Fountain watched her father go to medical school and become a doctor in the 1960s – a time when there were segregated professional organizations for physicians. The American Medical Association only admitted white doctors, and the National Medical Association was its counterpart for Black doctors. Being excluded from the AMA came at a cost: doctors weren’t allowed to practice in certain hospitals.
Public pressure during the Civil Rights movement ultimately forced the AMA to open its membership to everyone, regardless of skin color – and in 2008 the AMA issued a formal apology to Black doctors in the National Medical Association.
Today, Gibson Fountain serves as the American College of Obstetricians and Gynecologists representative to the American Medical Association. Her work in policy development benefits patients of every background across the country.
In addition to leading national policy development, she serves on local organizations including the Michigan Maternal Mortality Surveillance Committee, the Michigan Council for Maternal and Child Health, and the Southeast Michigan Perinatal Quality Improvement Coalition.
“Empathy has to be embedded in care,” Gibson Fountain said. “We have to change people’s minds. We have to change laws and change institutions. We have to hold people accountable for what happens. If we can’t touch your heart and mind, institutions have to hold people accountable.”
Blue Cross’s role
Blue Cross Blue Shield of Michigan is committed to helping to improve the health of all Michigan residents and is working to address health and health care disparities through policies, programs and initiatives.
Through the Health Disparities Action Team, formed in 2016, and the Office of Health and Health Care Disparities, formed in 2020, Blue Cross has convened stakeholders across the enterprise to implement a health equity lens across all of our work. This work is guided by data, listening to community members about their health care concerns and needs, as well as insight received from the Blue Cross’ Physician Diversity Council. The council was formed to address bias, health equity, representation in the provider community, cultural competency, gaps in resources and access for providers serving underserved communities – as well as other issues that influence health care access, quality and outcomes. Blue Cross has also offered unconscious bias education to providers across Michigan.
Blue Cross and the Blue Cross Blue Shield of Michigan Foundation closely track how social determinants of health affect the individuals in communities across the state, targeting grants and funding to organizations engaged in work on the ground that helps people bridge gaps and break down barriers when it comes to taking care of themselves, their families and their health.
Learn more about how Blue Cross is ready to help address health and health care disparities here.
Photo credit: Courtesy photos
Read on:
- Detroit R&B Artist Shines Despite Rare Case of Multiple Sclerosis
- Magnesium Supplements Are Trendy for Sleep and Anxiety. Are They Good For You?
- What is Night Eating Syndrome?