What to Know about Congenital Heart Defects in Infants
Jake Newby
| 3 min read
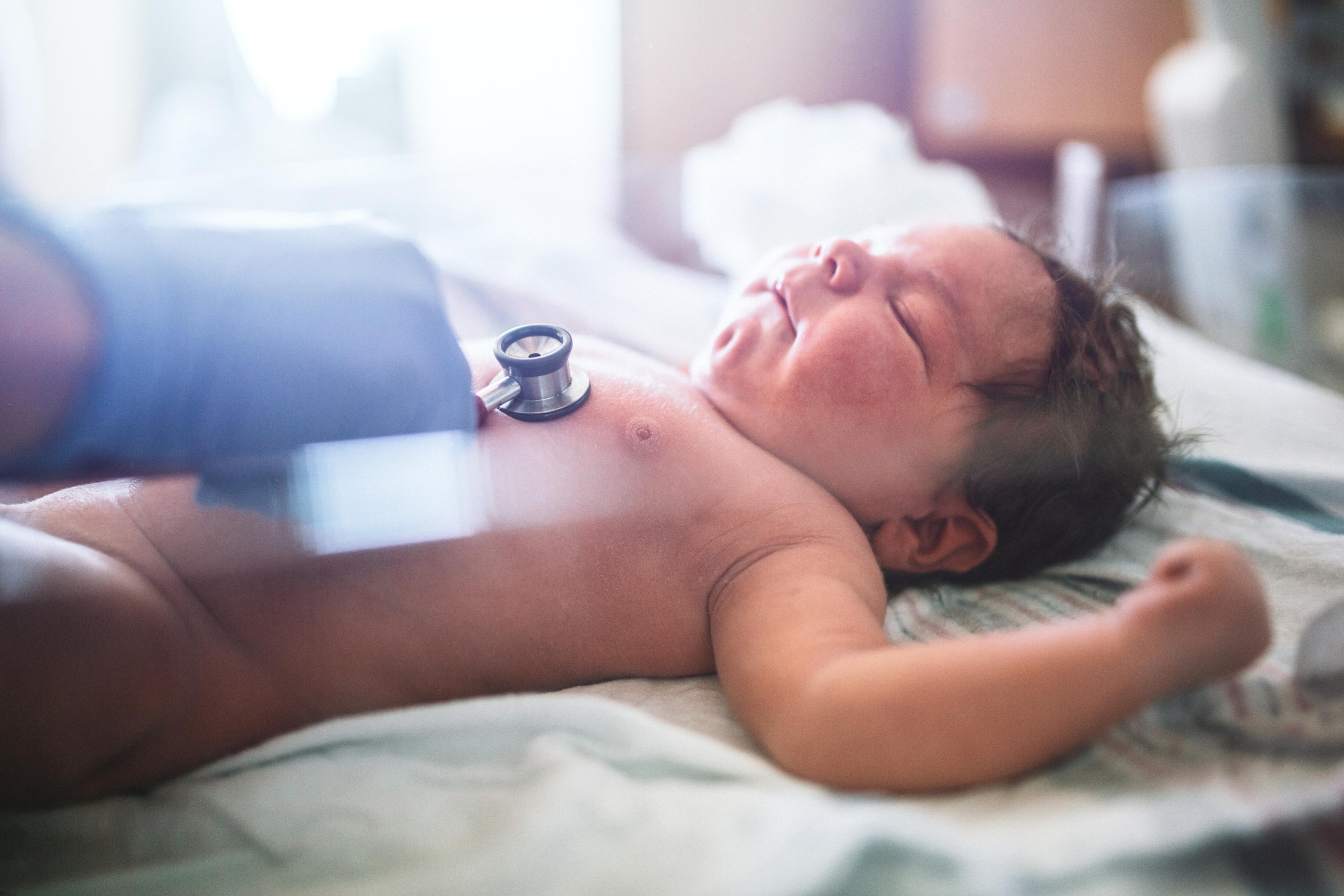
Congenital heart defects (CHD) – the most common type of birth defect – affect one out of every 110 infants born in the United States each year. That’s a total of 40,000 infants per year. The word “congenital” means that the problem existed or was present at birth. Sometimes, defects are detected during pregnancy. Other times, they are not detected until later in life, even adulthood.
CHDs affect the structure and functionality of the heart. They can involve abnormalities in the arteries, chambers, valves, or walls separating the chambers of the heart. CHDs also affect how blood flows through the heart and the rest of the body, and how oxygen flows to the lungs.
Signs and symptoms of congenital heart defects
Some CHDs – such as a small hole in the heart – can cause few problems. But in more severe cases immediate care is required. About one in four infants born with a heart defect has a critical CHD (also known as critical congenital heart defect). Infants born with a critical CHD need surgery or other procedures in their first year of life.
When CHD symptoms do occur in infants, they can include cyanosis, which is a pale gray or blue skin color. Since babies require a lot of effort to eat, eating can bring out symptoms of CHD including:
- Difficulty feeding
- Poor weight gain
- Rapid breathing and shortness of breath
Here are symptoms in older children:
- Fainting during exercise or physical activity
- Swelling in the hands, ankles, or feet.
- Tiring easily or experiencing shortness of breath
Congenital heart defect treatment
CHDs can be diagnosed in many ways. During pregnancy, a special type of ultrasound called a fetal echocardiogram may be used to generate ultrasound pictures of a developing baby’s heart. Other methods include:
- Pulse oximetry measurement
- Electrocardiogram
- Echocardiogram
- Chest X-Ray
- Cardiac MRI
- Cardiac catheterization
Not every child with a CHD requires active treatment. Small holes in the heart may go away on their own without treatment. Some conditions will require treatment like medications to control blood pressure, heart rhythm, or to remove excess water in the body.
More severe CHDs may require a surgical procedure to repair the defect. In cases where repairs aren’t an option, a heart transplant may be necessary, though this is an extreme measure that’s only recommended when all other options fail.
Living with a CHD
It is estimated that more than two million individuals in the United States live with CHD, many of whom live independent lives with little to no difficulty. This is credited in large part to advances in medical care and treatment.
For parents of children with CHDs, it is important to familiarize yourself with your child’s condition. Keep an eye out for worsening or new symptoms and be aware of any lifestyle adjustments recommended by your cardiologist.
As they age, individuals with a CHD can develop other health problems, depending on the type and severity of their heart defect. It is crucial for patients with a CHD to schedule routine checkups with a cardiologist (heart doctor) who has training in congenital heart disease.
Photo credit: Getty Images