Collaborative Care Addresses the Surging Demand for Mental Health Care Services
Deborah Reinheimer
| 3 min read

It’s not an exaggeration to say there is a mental health crisis in the United States. The need for mental health services continues to rise, particularly in a post-pandemic landscape. More than one-third of adults say they have a diagnosed mental health condition, a 5% increase from 2019 – with anxiety and depression being the most reported condition, according to the American Psychological Association.
In February 2021, 39.9% of adults in Michigan reported symptoms of anxiety or depression. Unfortunately, 27% reported being unable to receive the needed counseling or therapy.
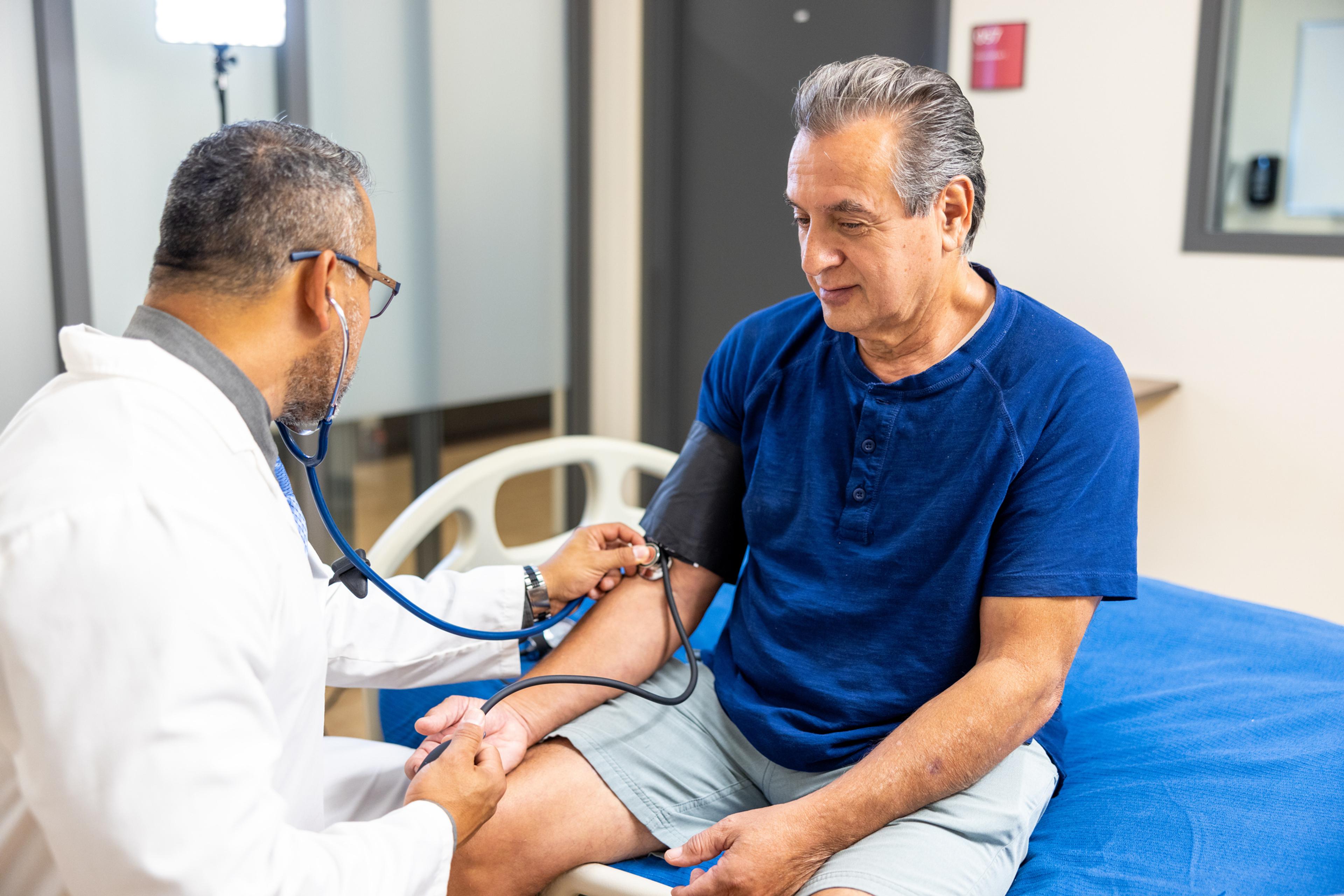
With the rise in anxiety and depression, the Collaborative Care program offers a solution. In the Collaborative Care model, primary care practices integrate mental health services into their practices. Patients have quicker, more direct access to behavioral health specialists through the same office where they receive regular health care.
The primary care physician works with a mental health care worker and a consulting psychiatrist to develop a mental health plan that fits each patient’s needs.
"This model of Collaborative Care allows for patients and primary care providers to have access to psychiatric recommendations promptly and in a less stigmatizing way. I love how we work as a team to help patients receive the most effective care,” said Dayna Le Platte, M.D., a consulting psychiatrist with the Collaborative Care program. “There is a shortage of mental health providers, and this model makes mental health more accessible. If someone has a mental health concern, they can continue to stay in [the primary care office] and get the evidence-based care that they need.”
Blue Cross Blue Shield of Michigan began working with physician organizations across the state a few years ago to develop and implement the Collaborative Care program. In September 2022, Blue Cross announced Collaborative Care designations for 213 physician practices, located in 33 counties throughout the state, including the Upper Peninsula. In 2023, that expanded to 239 primary care and 5 obstetrics/gynecology practices earning designation.
Designated practices have put systems in place to evaluate, treat and monitor patients’ mental health within the practice. This is part of the progression to team-based care influenced by the BCBSM Value Partnerships program. Value Partnerships is a collection of initiatives that improve health care quality and outcomes.
Ashley McClain, LMSW, supervises the Collaborative Care program within Michigan Medicine physician practices, and has witnessed great success from the care model.
“We’re able to provide another level of support to patients,” she said. “They’re learning coping strategies, behavior activation, different things they can do. They can be lifelong-changing interventions. I’ve had patients just thank us for the support we’ve been able to get them from the program.”
Learn more about how Blue Cross is ready to help support members and the community with mental health care here.
Learn more about Value Partnerships and its 20 years of health care excellence here.