What is a Pain Scale?
Amy Barczy
| 3 min read
Amy Barczy is a former brand journalist who authored content at Blue Cross Blue Shield of Michigan. Prior to her time at Blue Cross from 2019-2024, she was a statewide news reporter for MLive.com. She has a decade of storytelling experience in local news media markets including Lansing, Grand Rapids, Holland, Ann Arbor and Port Huron.

More than one in five American adults reported they experience pain most days or every day. Measuring pain is tricky: what is considered severe pain to one person could be mild pain for another person. It’s a subjective feeling. How do health care providers know what treatment to prescribe, if everyone perceives pain differently? Enter the pain scale. It’s a tool used to help patients report to doctors the pain they are feeling. Pain can be acute – meaning it goes away after treatment – or chronic, which means it is persistent. Pain that’s not managed correctly can contribute to worse physical and psychological outcomes for patients, as unrelieved pain stresses multiple systems in the body.
Types of pain scales
The most common type of pain scale measures how intense pain is. Here are some pain scales you may see in practice:
- Numeric rating scale: This uses a 1 to 10 scale to allow patients to rate their pain. Zero is considered no pain; 1 to 3 is mild pain; 4 to 6 is moderate pain and 7 to 10 is severe pain.
- Visual analog scale: This uses a continuous line, with one end marked as “no pain” and the other end marked as “worst possible pain.” Patients then are asked to mark a spot on the line to show their pain intensity, and doctors then determine a pain score.
- Categorical scale: In place of numbers, this scale uses words to indicate their pain. One end of the scale is “no pain” to “mild pain,” with the other end of the scale marked with “very severe pain” and “worst possible pain.” A version of this scale, known as the Wong-Baker Faces Scale, is used for children that uses graphic faces; “no pain” has a smiling green face, with a red crying face for “hurts worst.”
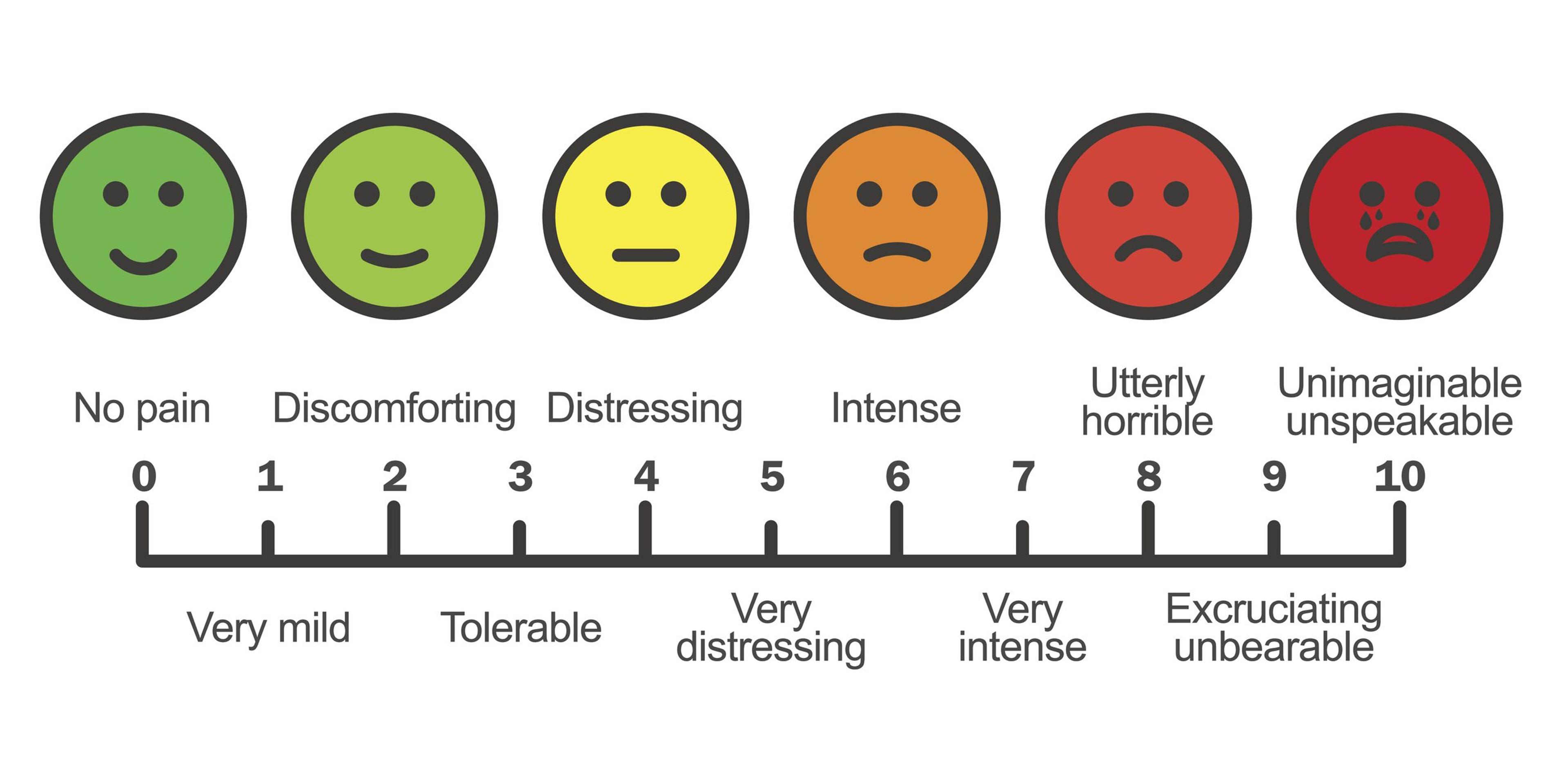
An example of a pain scale. Credit: Getty Images. Other pain scales are considered multidimensional, as they incorporate factors other than intensity of pain. Multidimensional pain tools are less commonly used. They can include initial pain assessment tools, the brief pain inventory and the McGill pain questionnaire.
How pain scales are used
Pain scales are a simple, quick way for doctors to understand what a patient is feeling. They work best when evaluating new, sudden pain. They can assist in prescribing treatment, as well as monitoring if treatment is effective. The goal of any treatment plan for pain is to make pain more manageable, not stop pain entirely. Patients may encounter a pain scale during a wellness checkup with their primary care provider, during admission to the hospital, before and after a surgery, or during physical therapy. Evaluating pain is considered by many in the medical field to be the “fifth vital sign,” in addition to body temperature, pulse rate, respiration rate and blood pressure. Pain is subjective; and pain scales attempt to relay the severity of pain for the individual to the providers so they know what the person is experiencing in the moment. Pain can have many influencing factors, especially if someone is experiencing chronic pain. If you’re experiencing long-term pain, talk to your health care provider. More from MIBluesPerspectives.com:
- The Evolution of Pain Management
- How to Safely Clean Out Your Medicine Cabinet
- How to Get a Narcan Kit in Michigan
Photo credit: Getty Images





